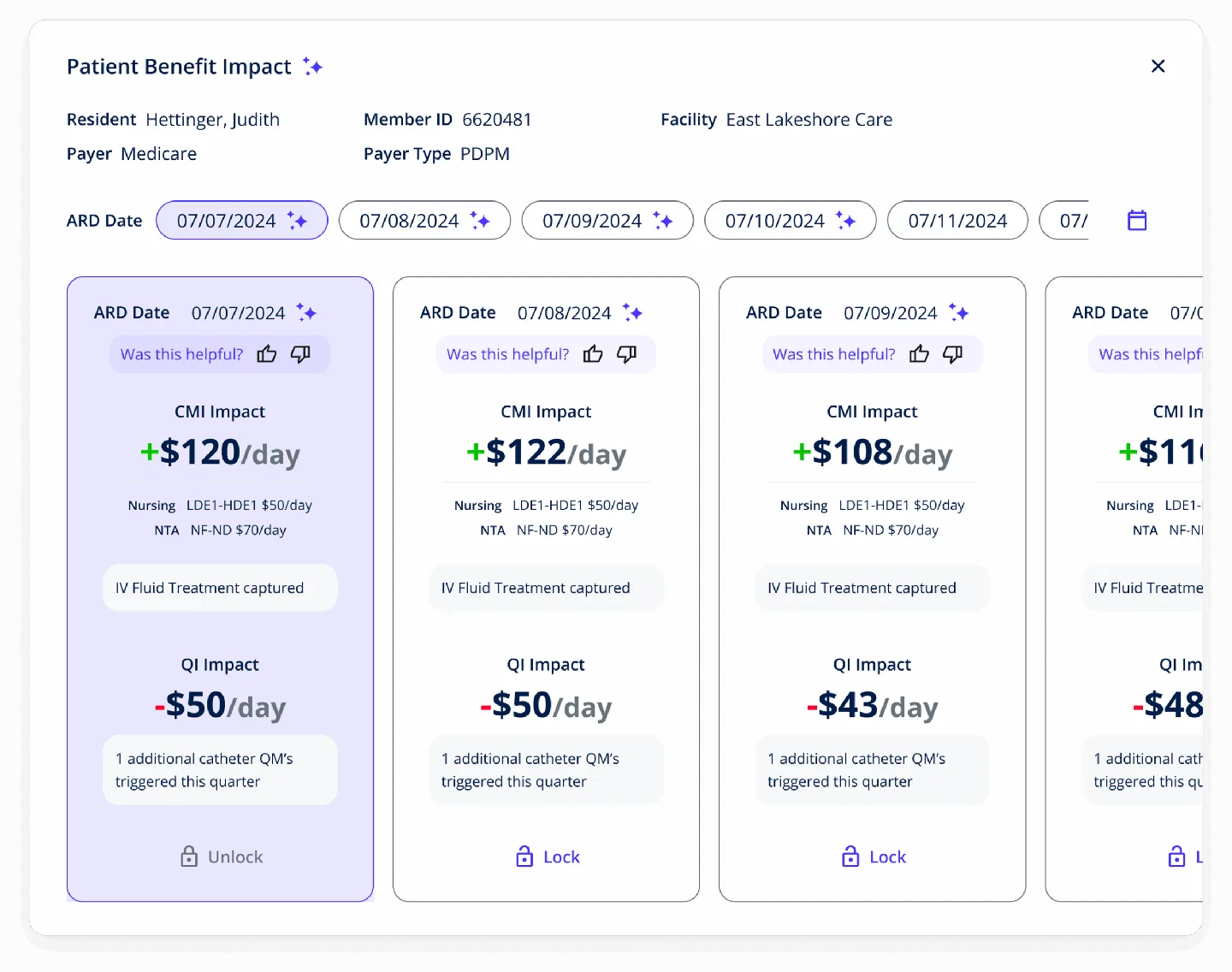
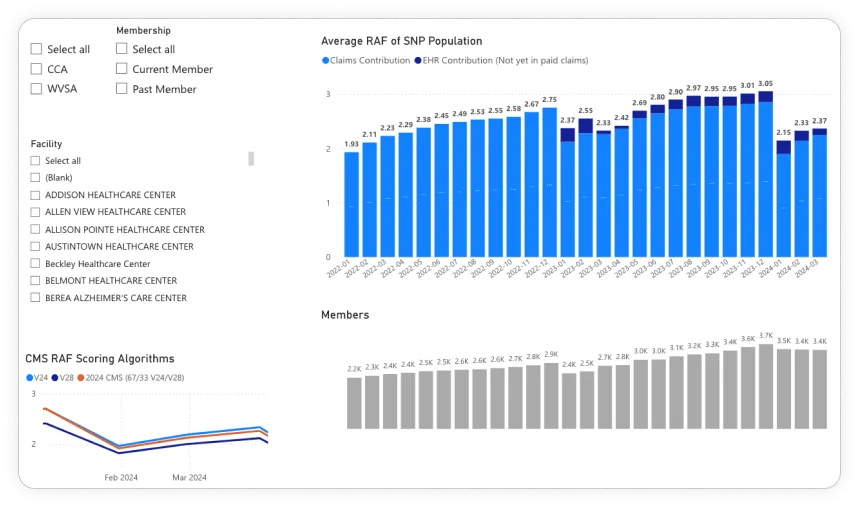
From system complexity to scalable value-based care
How Digital Scientists partnered with CommuniCare Advantage to eliminate technical debt across 60+ digital products, modernize their EHR ecosystem, and return the organization to CMS compliance — enabling both stability and growth.

Overcoming system complexity to achieve profitability
CommuniCare Advantage, a Medicare Advantage plan owned by the CommuniCare Family of Companies — a $2B leader in post-acute healthcare — was expanding into an Accountable Care Organization while being weighed down by excessive and outdated technology solutions across 60+ digital products. The transition required a modern approach to value-based care.
Digital Scientists provided technical architecture consulting to audit their entire technology ecosystem, identify and eliminate technical debt, manage a comprehensive EHR vendor selection process, and deliver a unified data and reporting solution through PowerBI — returning the organization to compliance in under six months and positioning them for sustained growth. Our deep experience with EHR integrations and interoperability was central to the engagement. For organizations evaluating a similar transformation, this is the kind of work we deliver as a healthcare app development partner.
“Digital Scientists provided immense value to our plan administrators, providers, and patients. The team was able to come in and understand our core needs, while remaining product agnostic. They helped identify the technical debt and pitfalls, and to get us to a point of stabilization and growth.”
Robert Hager
CEO, CommuniCare Advantage
<6mo
Returned to CMS compliance
25%
Technology footprint reduction
20%
Yearly growth potential
60+
Digital products audited
Rapid growth met by mounting technical debt
CommuniCare Advantage was expanding beyond a traditional Medicare Advantage plan to also become an Accountable Care Organization (ACO). But years of acquisitions and organic growth had created a fragmented technology ecosystem that was holding the business back.
Disconnected Systems
Over 60 digital products across the organization, many outdated and out of sync. No single source of truth for clinical, compliance, or operational data.
- Multiple EHR platforms not meeting growing needs
- Siloed data across clinical and operational systems
- Technology ecosystem creating cost, not revenue
Compliance at Risk
CMS Medicare Advantage regulations require rigorous data reporting and visibility. Without consolidated systems, the organization was at risk of non-compliance and missed reimbursements.
- CMS audit requirements not fully met
- Declining reimbursements from under/missed billing
- No proactive visibility into operational data
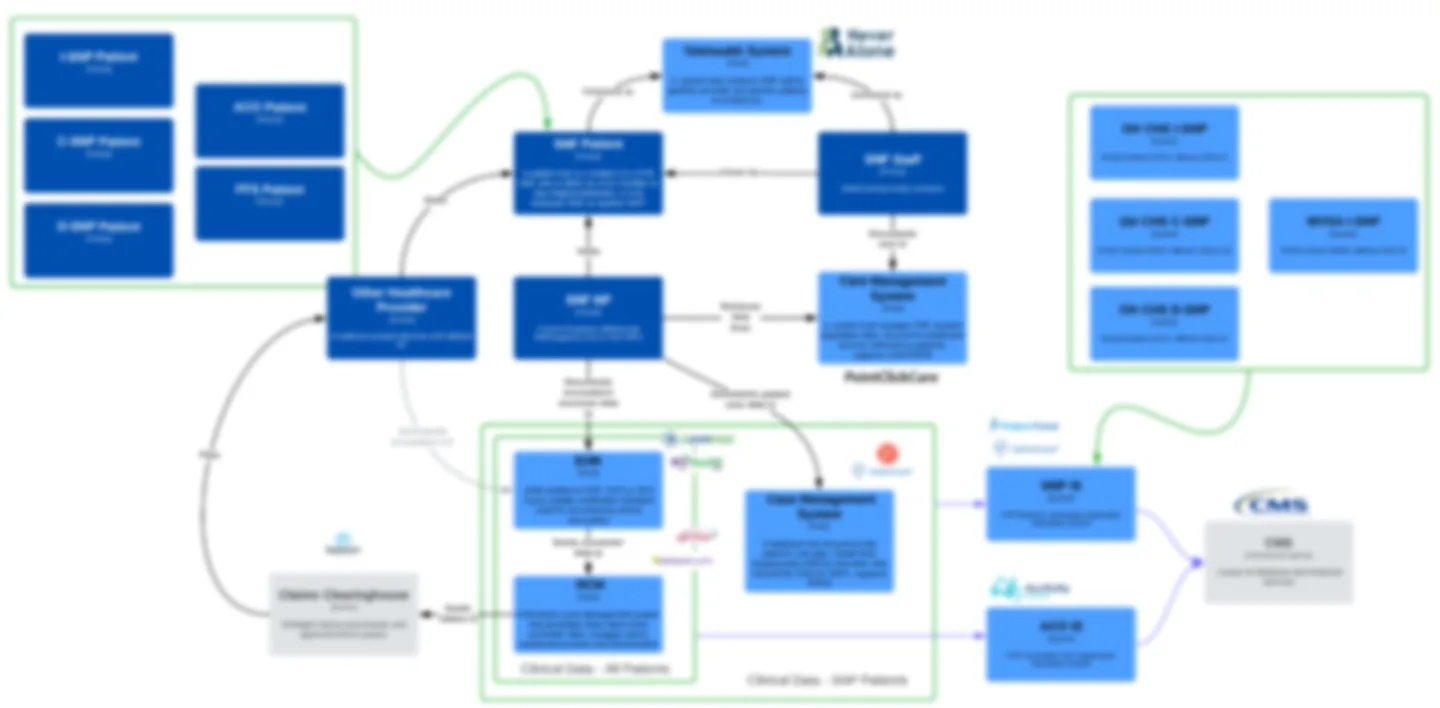
Technology ecosystem audit — mapping 60+ digital products and their dependencies
From technical debt to maximized revenue
Through continuous delivery and pragmatic consulting, we focused on what would bring the most value to our client across a 15-month engagement.
Q4 2022
User + System Research
Q1 2023
Digital Ecosystem Audit
Q1 2023
Ecosystem Map Deliverable
Q1 2023
Landscape Analysis
Q2 2023
RFP + Implementation
Q3 2023
Reporting Solution Deliverable
Q4 2023
Final Results
A structured three-phase engagement
Discovery & Assessment
- Executive-level user interviews
- Subject matter expert interviews
- Technology ecosystem audit (60+ products)
- Current & future state ecosystem maps
- Compliance requirement documentation
Analysis & Design
- EHR landscape analysis (11 vendors)
- Buy, build, partner framework
- RFP development & vendor management
- Grading matrix for vendor evaluation
- Data integration strategy
Implementation
- Consolidated data mart (single source of truth)
- PowerBI reporting suite
- EHR migration consultation
- Gap analysis of chosen platform
- Training & knowledge transfer
Turning technology into a revenue driver
The product and solution architecture team from Digital Scientists approached CommuniCare Advantage’s issues with the deep desire to understand their problems, their ecosystem architecture, and the future state they needed in order to help their growing business thrive.
Technology Ecosystem Audit
Comprehensive assessment of 60+ digital products — identifying what was working, what was not, and what was critical to the business
EHR Vendor Selection & RFP
Landscape analysis of 11 EHR platforms, formal RFP process with grading matrix, managed vendor communications and onsite presentations
Data Consolidation & PowerBI
Unified all data sources into a single SQL data mart, built a comprehensive PowerBI reporting suite covering compliance, operations, and clinical metrics
Compliance Reporting
Universe Report (CMS Audit), HRA completion reports, ICT/ICP completion reports, risk level reports, scheduling reports, and operational dashboards
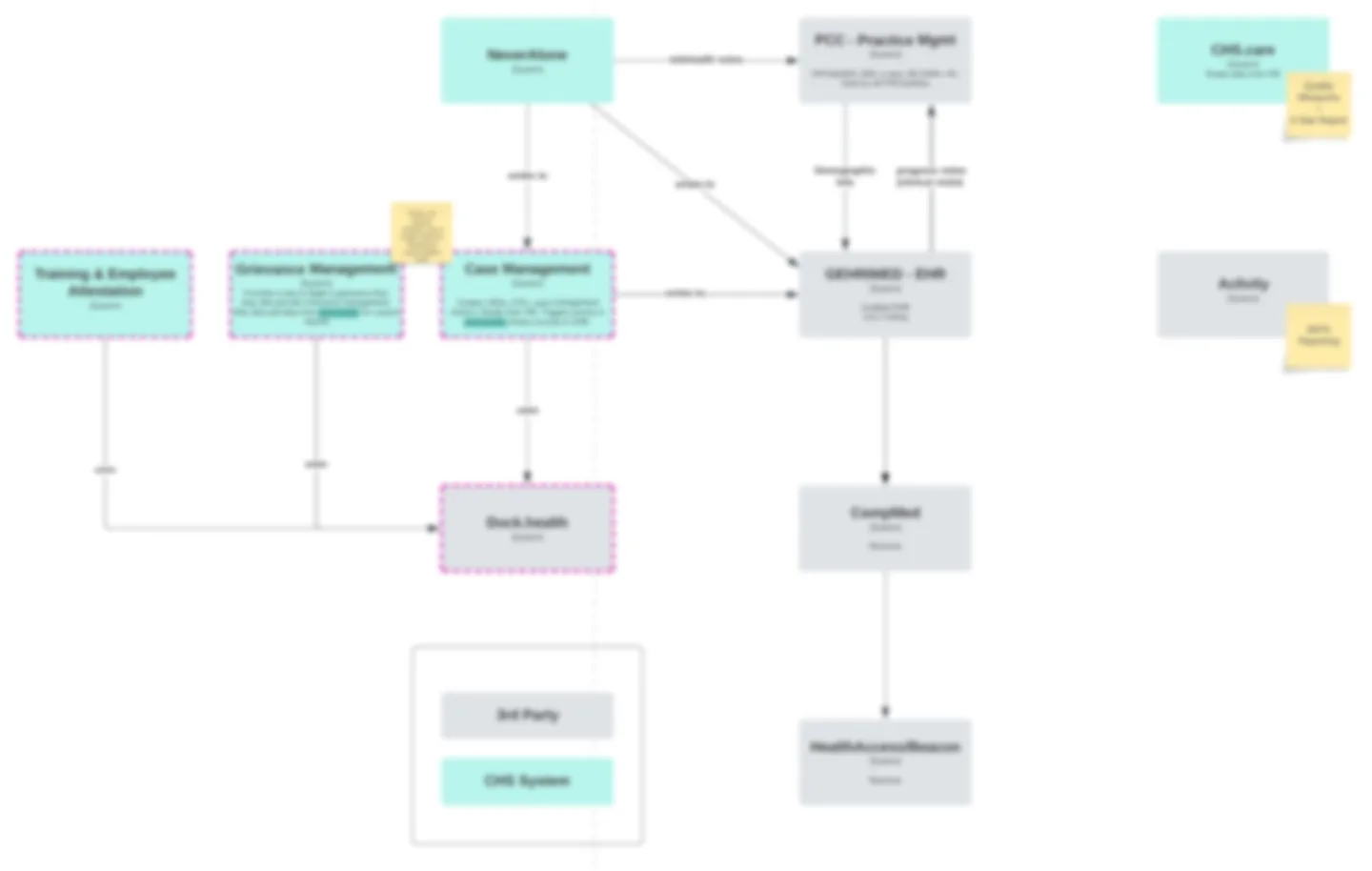
Future state ecosystem architecture
Finding the right platform to scale
We performed a qualitative assessment of eleven Electronic Health Record and clinical case management solutions based on system requirements, post-acute care expertise, compliance capabilities, and integration potential.










434 requirement items evaluated across 15 functional categories
From technical debt to proactive growth
Compliance Visibility
A single source of truth through a consolidated Data Mart ensures real-time visibility into data, allowing proactive reporting for ongoing CMS compliance. Leadership, plan administrators, and providers can access their data at any time.
Modernized EHR
Through a repeatable, scientific method of product strategy, we guided the selection and migration to a stable, modern EHR that integrates with the existing ecosystem and ensures provider adoption.
Revenue Growth
By reducing technical debt and removing unnecessary platforms, we ensured the EHR would reduce under/missed billing through intuitive workflows — positioning the organization for 20% yearly growth potential.
Hear from the CEO
Robert Hager, CEO — CommuniCare Advantage
More with CommuniCare
Struggling with healthcare IT complexity?
We help healthcare organizations eliminate technical debt, modernize their technology ecosystems, and build for scale. Let’s talk about your challenges.