$10M PDPM revenue recovered. $2M in quality incentives.
CommuniCare Health Services—one of the nation’s largest post-acute care providers—needed to optimize MDS assessments across their skilled nursing facilities. We built AI-powered tools that transformed PDPM revenue capture while improving quality scores.
 Click to zoom
Click to zoom
PDPM Revenue Recovered
Quality Incentives (Annual)
Five-Star QM Score
Time Savings Per Assessment
AI-powered MDS optimization at national scale
CommuniCare Health Services needed to optimize MDS assessments across their skilled nursing facilities. Manual reviews took 3–4 hours per resident, and uncaptured diagnoses were directly impacting PDPM reimbursement and quality scores.
Digital Scientists built an AI-powered coding engine that ingests data from six clinical sources to surface uncaptured ICD-10 codes with confidence scoring and clinical evidence linking—reducing review time from hours to roughly 60 seconds per patient. Learn more about our approach to MDS optimization and PDPM revenue capture.
The platform has expanded to include ARD optimization (expected ~$20M additional annual impact), event scanning across 200+ clinical triggers, multi-facility operator dashboards, PCC real-time integration, and regulatory compliance automation. It is a prime example of our revenue cycle AI solutions in action.
Millions in revenue leakage from incomplete MDS assessments.
CommuniCare’s MDS coordinators were drowning. Each assessment took 3–4 hours, and with hundreds of residents across multiple states, diagnoses were going uncaptured, directly impacting PDPM reimbursement.
The problem wasn’t competence—it was capacity. Coordinators didn’t have time to review every clinical note, lab result, and medication record for every resident. Diagnoses were going uncaptured. Revenue was walking out the door.
Before DS
3–4 hours per MDS assessment
Manual review of clinical documentation, medications, lab results
Uncaptured diagnoses at scale
Not enough time to catch everything buried in the chart
Revenue leakage at scale
Hundreds of residents, millions in missed reimbursement
Quality scores suffering
Incomplete documentation affecting Five-Star ratings
We mapped the entire MDS ecosystem before writing code.
Before building anything, we conducted deep persona research to understand the MDS nurse’s world—their workflows, tools, challenges, and the network of stakeholders they coordinate with daily.
The MDS Coordinator
Also known as: MDS Nurse, RAI Coordinator, MDS Assessment Nurse, Clinical Reimbursement Specialist, PDPM Coordinator
Distinguished by dedication to quality resident care, trained in MDS assessments, synthesizes large quantities of data from resident interviews, health records, and clinical documentation.
Jobs to Be Done
- • Ensure accurate, comprehensive resident assessments reflecting clinical acuity
- • Identify and respond to significant changes in resident status promptly
- • Adhere to RAI guidelines, ARD timelines, and state MDS regulations
Tools & Devices
PointClickCare (PCC), printed health records, laptop w/dual monitors
Key Challenges Uncovered
Documentation & data accuracy
Inaccurate coding, data entry errors, and incomplete documentation due to inconsistent, unavailable data or overwhelming information volume. Reliance on printed records makes verification time-consuming and error-prone.
Selecting the correct ARD date
Requires extensive RAI manual knowledge, years of experience, and excellent judgment—balancing precise care planning with optimal financial reimbursement amidst potential audits.
Coordination across disciplines
MDS nurses coordinate with nursing staff, physicians, therapists, dieticians, social workers, and admissions nurses—communication gaps and scheduling conflicts lead to assessment discrepancies.
Stakeholders Mapped
8
Roles across the MDS ecosystem
Shadowing
40+
Hours with MDS coordinators
User Interviews
17+
Facility & workflow validation
Feedback Loops
Weekly
Hotjar + champion nurse sessions
AI-powered MDS assistant built with—not for—MDS coordinators.
We didn’t build an algorithm and hand it over. We embedded with CommuniCare’s MDS team, shadowed their workflows, and co-designed a solution that actually fit how they work.

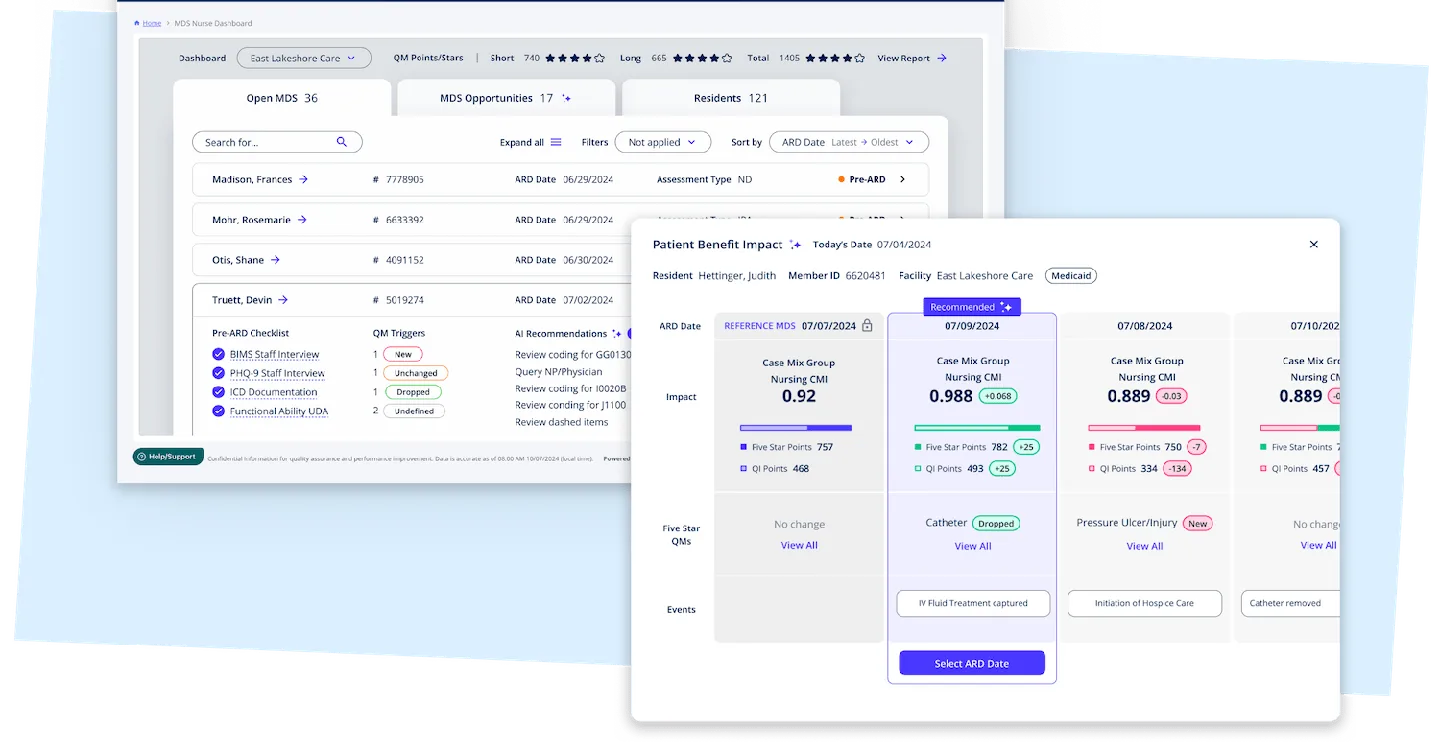
AI Diagnosis Recommendations
Our AI reviews clinical documentation, medications, and lab results to surface diagnoses that should be captured on the MDS. Every recommendation linked to supporting documentation—audit-ready from day one.

Pre-Submission Validation
Before MDS submission, AI flags potential errors, uncaptured diagnoses, and inconsistencies. Catch problems before they become denials or audit findings.
 Click to zoom
Click to zoom
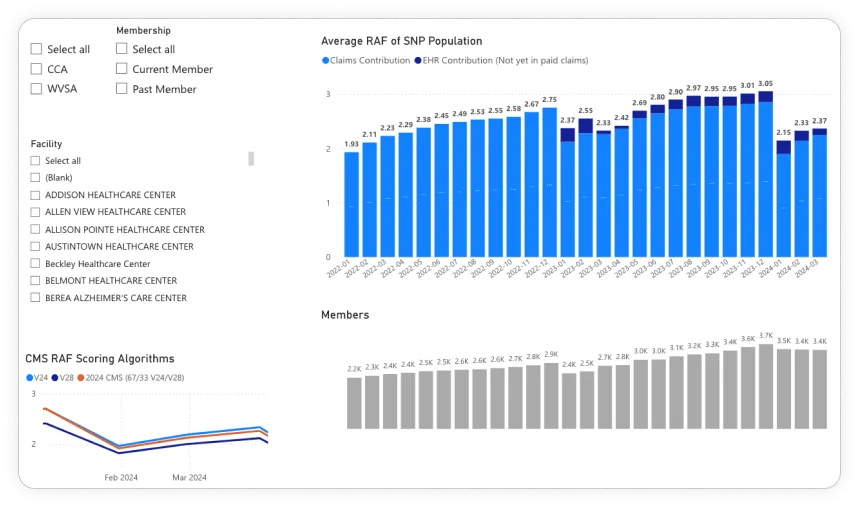
Quality Analytics
Real-time visibility into quality measure performance across facilities. Identify improvement opportunities, track progress, and prepare for surveys.
Actionable insights at every level
Each facility gets a dedicated overview showing quality score trends, CMI averages, total residents by status, and actionable alerts sorted by urgency. Operators can drill from regional overview to individual resident in seconds.
 Click to zoom
Click to zoom
Every resident, every deadline
The resident list gives MDS nurses at-a-glance status for every resident—overdue, due within 14 days, in progress, or discharged. Quick filters surface the most urgent work, and one click opens the full resident summary.
 Click to zoom
Click to zoom
Detecting opportunities before they expire.
The system continuously scans clinical data to detect events—falls, new diagnoses, weight changes, isolation, and 200+ other triggers—that create MDS optimization opportunities. Each event is tied to a look-back period, and the ARD optimizer quantifies the financial impact of choosing different Assessment Reference Dates.
 Click to zoom
Click to zoom
Event Detection with Evidence
Each detected event surfaces the source data—physician orders, progress notes, lab results—so nurses can verify the finding and decide on action. Events that affect PDPM or quality measures are prioritized by urgency and look-back window.
 Click to zoom
Click to zoom
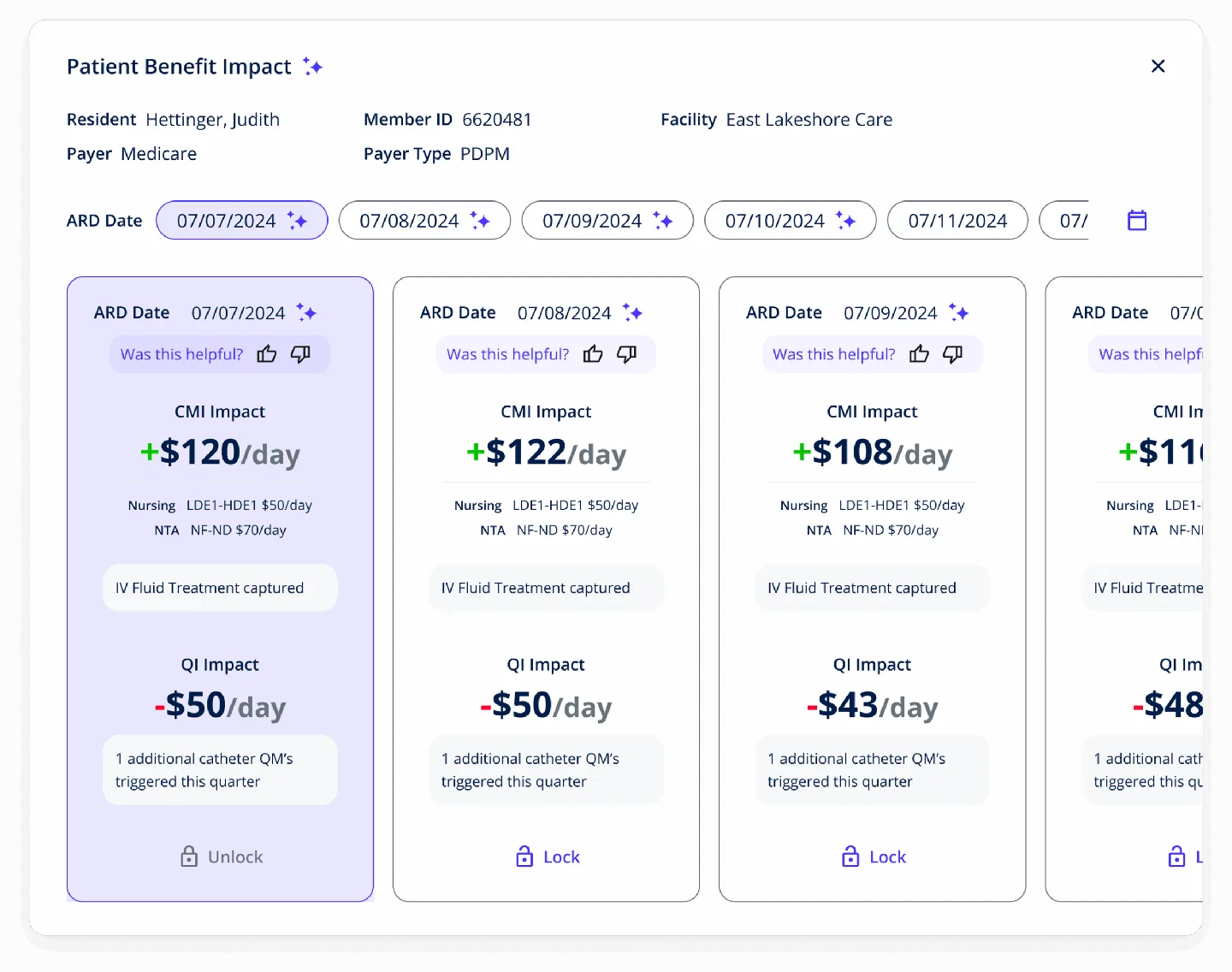
ARD Optimization
Nurses can evaluate multiple ARD dates side-by-side, seeing the impact on Nursing CMI, case mix group, and Five-Star quality measures. In complex cases, higher payment can compete with quality ratings—the system helps nurses make the best decision for both the resident and the facility.
Five-Star performance at your fingertips
The platform tracks 10+ quality measures in real time, showing numerators, denominators, current points, and Five-Star ratings for both short-stay and long-stay residents. Facilities can see exactly where they stand and where opportunities exist.
Quality score trends over time show the impact of optimization efforts, with CMI averages tracked monthly. This data drives both clinical decisions and financial planning.
 Click to zoom
Click to zoom
How the complete value chain delivered $12M+ in results.
This wasn’t just an AI project. It was a complete transformation—from messy data to measurable outcomes. Here’s how each step contributed to success.
Data Foundation
Integrated clinical data from PointClickCare across multiple facilities. Cleaned and structured medication records, lab results, and clinical notes into AI-ready format.
Responsible AI Build
Built AI using peer-reviewed CMS scoring models. Every recommendation explainable and linked to source documentation. 90%+ diagnosis accuracy validated.
EHR Integration
Seamless PointClickCare integration. AI recommendations surface within existing workflow—no separate login, no duplicate data entry. Real-time validation before CMS submission.
Co-Design
40+ hours shadowing MDS coordinators before writing code. Persona research across 8 stakeholder roles. Weekly feedback sessions throughout development.
Implementation
Phased rollout starting with pilot facilities. June 2025 Verify release. On-site go-live support. Rapid issue resolution. No “deploy and disappear.”
Change Management
Training programs for MDS coordinators. Champion nurse identification. Hotjar surveys and user interviews. Adoption from day one—not months later.
Regulatory Automation
AI agents monitor CMS regulatory sites for changes. Versioning framework ensures MDS logic always uses the latest published rates, guidelines, and RAI manual updates.
Ongoing Partnership
Regular executive reviews. Continuous optimization based on CMS updates and facility feedback.
ARD optimization: the next ~$20M opportunity
ARD date optimization analysis identified substantial additional reimbursement opportunities across facilities by surfacing cases where alternative Assessment Reference Dates would yield higher PDPM payments.
The analysis dashboard captures PDPM payment differences, nursing CMI comparisons, and quality measure impacts—giving operators clear visibility into the value of optimization.
 Click to zoom
Click to zoom
Validated against actual performance data.
Results validated against actual PDPM reimbursement and quality performance data.
Financial Impact
Annualized. Previously uncaptured diagnoses now surfaced through AI-powered recommendations.
Annual quality incentive payments earned through improved quality measure performance.
Additional annual earnings from ARD date optimization across facilities.
Per patient benefit from more accurate case mix index classification.
Operational Impact
MDS coordinators spend less time hunting through charts, more time on clinical judgment.
Quality measure performance improved through better documentation and coding accuracy.
AI recommendations validated against clinical documentation with high accuracy.
Clinical triggers monitored continuously, with expanded data sources and benchmarked accuracy.
40+ hours shadowing before writing code.
Most healthcare AI projects fail because they’re built in conference rooms, not clinical settings. We took a different approach.
We embedded with MDS coordinators
Before writing a single line of code, our team spent 40+ hours shadowing MDS coordinators. Watching their actual workflow. Understanding their pain points. Learning their language. We mapped 8 stakeholder roles across the MDS ecosystem.
We built for audit defense
Every AI recommendation is linked to supporting clinical documentation. When auditors ask “why did you capture this diagnosis?”—there’s an answer ready. Defensible from day one.
We drove adoption, not just deployment
Change management isn’t an afterthought. We trained coordinators, identified champion nurses, launched Hotjar surveys and user interviews, and addressed resistance head-on. The solution works because people actually use it.
What’s your MDS optimization opportunity?
If uncaptured diagnoses are costing you millions in PDPM reimbursement, let’s talk. 30-minute call to assess your opportunity.
Schedule Assessment CallRelated Insights
From Our Blog

Rebuilding the Essential Economy with AI Innovation
Jul 09, 2025

Managing Architecture and Telehealth to Combat the Rise of the Financial Crisis
Dec 12, 2023

An Essential Guide to Managing Software Development Risk and Maximizing ROI
Dec 23, 2025
Healthcare Technology
Ready to Transform Your Healthcare Technology?
We’ll scope a working prototype for your MDS optimization challenge in one week.
Since 2007 · 200+ products launched · One team, concept to scale