$10M+ in risk adjustment improvements. 90%+ diagnosis accuracy. 7 states.
A value-based care organization serving Medicare Advantage patients needed to improve risk adjustment accuracy. Missed HCC codes were leaving millions on the table. We built an AI-powered platform that transformed their RAF scores while reducing audit risk.
RAF Improvements
Diagnosis Accuracy
Patients Served
Providers
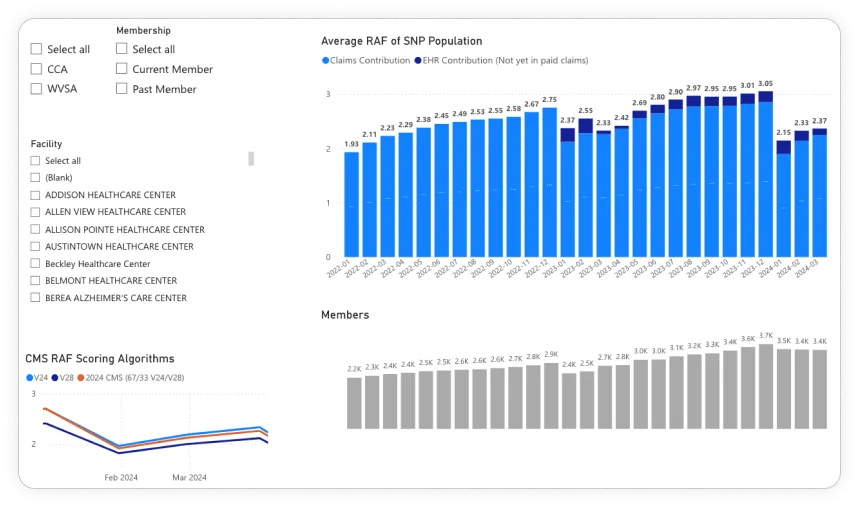
Millions in missed risk adjustment from incomplete coding.
In Medicare Advantage and value-based care models, accurate risk adjustment is everything. HCC codes determine payment rates. Missed diagnoses mean missed revenue-and inaccurate patient risk profiles that affect care planning.
This organization had a problem at scale: 20,000+ patients across 7 states, 245 providers, and no systematic way to ensure diagnoses documented in clinical notes were being captured in claims. The gap between documentation and coding was costing millions.
The Risk Adjustment Challenge
Documentation-to-coding gap
Diagnoses documented in notes but not making it to claims
Chronic condition recapture
HCCs from prior years not being recaptured annually
Audit risk
Coding without clear documentation linkage creates exposure
Scale complexity
20K+ patients, 7 states, 245 providers-impossible to review manually
AI-powered risk adjustment with explainable recommendations.
We built a platform that reviews clinical documentation-EHR data, lab results, medications, problem lists-and surfaces HCC coding opportunities with direct links to supporting evidence. Every recommendation is audit-defensible.
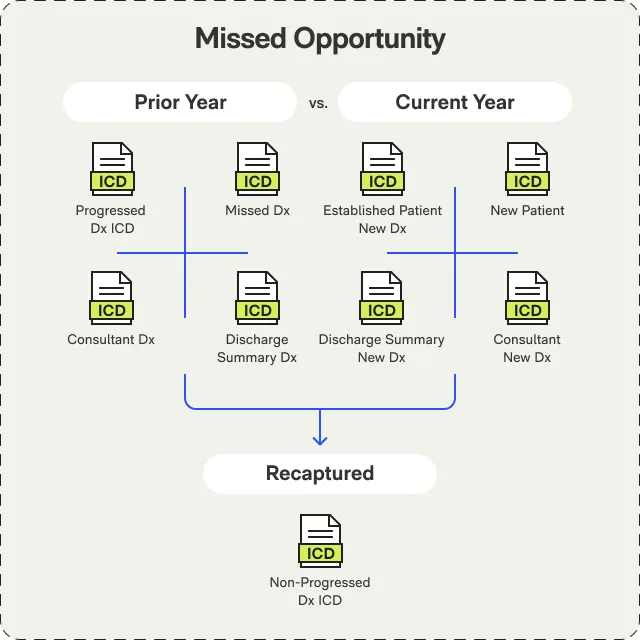
Holistic Patient Views
Unified view of each patient's clinical data across all sources-EHR, labs, medications, claims history. AI identifies HCC gaps by comparing documented conditions against coded diagnoses.
* Multi-source data integration (EHR, claims, labs, medications)
* Prior year HCC recapture identification
* Suspected condition flagging
* Clinical evidence linking
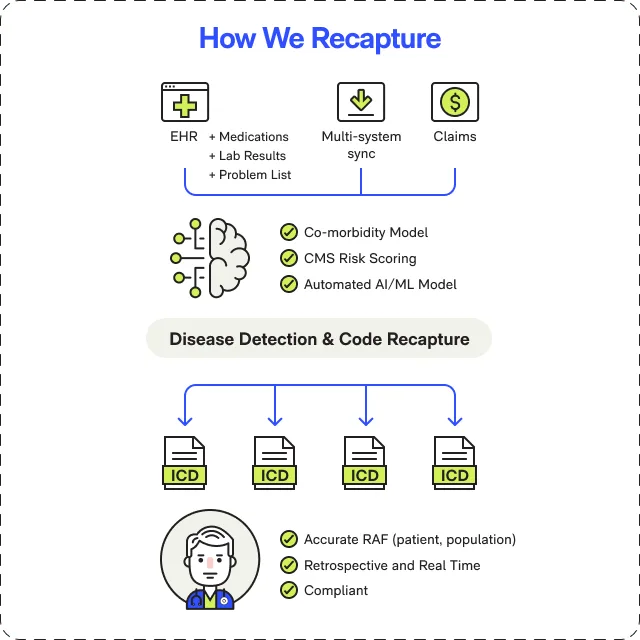
Provider Workflow Integration
Recommendations surface at the point of care, not in a separate system. Providers see HCC opportunities during the visit, with supporting documentation pre-populated.
* EHR integration (Gehrimed, PointClickCare, Acclivity)
* Pre-visit preparation reports
* In-visit prompts for missing HCCs
* One-click documentation support

Population Analytics
Enterprise visibility into RAF performance across facilities, providers, and patient populations. Identify systematic gaps, track improvement, and prioritize interventions.
* RAF score trending by facility
* Provider performance comparisons
* HCC gap analysis by category
* ROI tracking and forecasting
Audit-Ready Documentation
Every HCC recommendation linked directly to clinical evidence. When auditors ask "why did you code this?"-the answer is one click away. Built for defensibility.
* Source document linking
* Clinical evidence chains
* Audit trail logging
* Peer-reviewed CMS methodology
Responsible AI with explainability at the core.
Healthcare AI isn't just about accuracy-it's about explainability. Every recommendation must be defensible. We built this platform with auditability as a first-class requirement.
Peer-Reviewed Methodology
AI models built on CMS HCC scoring methodology. Not black-box predictions-transparent, validated approaches.
Evidence Linking
Every recommendation tied to specific clinical documentation. Auditors can trace from code to evidence in seconds.
Multi-Source Integration
EHR data, lab results, medications, claims history-all combined for comprehensive patient view.
Continuous Learning
Platform improves with feedback. Provider corrections and audit results feed back into the model.
$10M+ in improvements across 7 states.
Production deployment serving real patients, real providers, real revenue. These numbers come from actual RAF score improvements tracked over time.
Financial Impact
Total RAF improvements
ICD/HCC recapture rates
Audit exposure and claw-back risk
Clinical Impact
Diagnosis accuracy
Patient risk profiles for care planning
Hospitalizations through better targeting
Scale
Patients served
States in production
Providers using the platform
Wrapped around existing EHR systems.
No rip-and-replace. The platform integrates with existing EHR systems, pulling data for analysis and surfacing recommendations within provider workflows. Providers don't need to log into another system.
Production Integrations:
Gehrimed
Primary EHR integration
PointClickCare
SNF data integration
Acclivity
Claims and billing data
Lab Systems
Results integration
Why Integration Matters for RAF
Complete patient picture
Lab results, medications, and clinical notes all factor into HCC identification.
Point-of-care delivery
Recommendations surface during the visit, not in a separate report reviewed later.
No duplicate data entry
Providers accept or modify recommendations-data flows back automatically.
Audit trail preservation
Source documentation links maintained through the workflow.
More healthcare results.
What's your risk adjustment opportunity?
If missed HCCs are costing you millions in RAF revenue, let's talk. 30-minute call to assess your opportunity.
Schedule Assessment CallRelated Insights
From Our Blog

Leveraging AI tools in Social Need Screening and Intervention – comments on proposed changes to HEDIS SNS-E measure
Feb 19, 2025

AI & The Job Landscape, ChatGPT’s Role, & The Future of RPM
Dec 12, 2023
Leveraging AI for ROI in Healthcare: 10 Custom Solutions for 2026
Nov 28, 2025
Healthcare Technology
Ready to Transform Your Healthcare Technology?
We’ll scope a working AI prototype for your RAF/HCC coding challenge in one week.
Since 2007 · 200+ products launched · One team, concept to scale

