Ambient AI Scribes
Your clinicians spend 45 minutes per visit on documentation. That's time stolen from patient care-and the primary driver of burnout. Ambient AI scribes listen to clinical conversations and generate accurate documentation automatically. We build custom scribes that understand your specific documentation requirements.
Min Per Visit
More Patients/Day
Time Savings
Month Payback
AI-powered clinical documentation
AI that listens, understands, and documents
Ambient AI scribes use advanced speech recognition and natural language processing to capture clinical conversations in real-time. Unlike transcription services that produce raw text, ambient scribes understand medical context and generate structured documentation that fits your requirements.
The technology has matured rapidly. Speech recognition accuracy for medical terminology now exceeds 95%. More importantly, large language models can interpret clinical conversations-identifying diagnoses discussed, treatments recommended, and assessments made-and organize this information into compliant documentation.
But healthcare documentation isn't one-size-fits-all. OASIS assessments differ from MDS evaluations. Home health visit notes differ from SNF progress notes. Generic ambient scribes miss the mark. Custom solutions, trained on your specific documentation standards and integrated with your EHR, deliver real results.
How Ambient AI Scribes Work
Listen
AI captures the clinical conversation through mobile device, desktop, or dedicated hardware.
Understand
NLP extracts clinical information: symptoms, assessments, diagnoses, treatments, patient responses.
Generate
AI creates structured documentation in your format-visit notes, OASIS responses, care plan updates.
Review
Clinician reviews, edits if needed, and approves. Documentation flows to EHR.
Documentation burden is unsustainable
The documentation crisis affects every healthcare setting, but the burden varies by care type. Custom solutions address your specific challenges.
Per Visit Documentation
Clinicians spend more time typing than treating. This ratio is inverted from what it should be.
Daily Charting
Nurses and clinicians spend significant portions of their day on paperwork instead of patient care.
Burnout Driver
Documentation burden consistently ranks as the top contributor to clinician burnout and turnover.
Custom scribes for every healthcare setting
Each care setting has unique documentation requirements. Generic solutions miss the nuances. We build scribes tailored to your specific needs.
Home Health & Hospice
OASIS assessments, visit notes, care plan updates, medication reconciliation-generated from the natural flow of the home visit conversation.
- *OASIS assessment auto-population from visit conversation
- *Skilled visit note generation with intervention documentation
- *Care plan updates based on patient progress discussed
- *Medication reconciliation from verbal review
Skilled Nursing Facilities
Progress notes, shift documentation, MDS support, incident reports-voice-enabled documentation that works during rounds, not after.
- *Progress note generation from rounds discussion
- *Shift documentation for CNAs and nurses
- *MDS assessment support with clinical observation capture
- *Incident and event documentation
Outpatient & Primary Care
Office visit notes, HPI documentation, assessment and plan, orders-comprehensive documentation from the patient encounter.
- *Chief complaint and HPI from patient narrative
- *Physical exam documentation with findings
- *Assessment and plan with diagnoses and orders
- *Patient education documentation
Personal Care & Assisted Living
ADL documentation, observation notes, caregiver communication-simplified documentation for non-clinical staff.
- *ADL assistance documentation via voice
- *Behavioral observation notes
- *Meal and hydration tracking
- *Activity participation records
What makes our ambient scribes different
Medical-Grade Speech Recognition
Trained on healthcare terminology, medication names, diagnoses, and procedures. 95%+ accuracy for clinical vocabulary that generic speech recognition misses.
Clinical NLP Understanding
Not just transcription-understanding. The AI identifies clinical entities, relationships, and context to generate meaningful documentation.
Custom Documentation Templates
Output matches your specific documentation requirements. OASIS, MDS support, visit notes, progress notes-whatever format your organization uses.
EHR Integration
Documentation flows directly to your EHR-PointClickCare, Epic, Gehrimed, Elation. No copy-paste, no duplicate entry.
HIPAA Compliant
PHI handling built in from the start. Audio processing, data transmission, and storage all meet HIPAA requirements.
Continuous Learning
The system learns from corrections and feedback, improving accuracy for your specific clinicians, terminology, and documentation preferences.
The economics of ambient scribes
Documentation automation delivers clear, measurable ROI through time recovery and capacity expansion.
Time Savings
Documentation time drops from 45 minutes to 5 minutes per visit.
Additional Patients
Clinicians can see 2-3 more patients daily with the same working hours.
Capacity Unlock
Serve more patients without hiring additional clinical staff.
Payback Period
Investment typically pays back within the first year through capacity gains.
Often combined with
Documentation Automation
Ambient scribes are part of our broader documentation automation framework-including OASIS, MDS support, and care plans.
See framework →MDS / PDPM Optimization
Ambient scribes capture clinical observations that support accurate MDS assessments and PDPM reimbursement.
Learn more →EHR Integrations
Ambient scribes require seamless EHR integration to deliver value. We have production experience with major platforms.
Learn more →RAF / HCC Coding
Better clinical documentation from ambient scribes means more accurate diagnosis capture and risk adjustment.
Learn more →Revenue Cycle AI
Complete documentation at the point of care means cleaner claims and faster reimbursement downstream.
Learn more →AI frameworks that power this domain.
HealthContext.AI
AI-powered medical transcription reducing documentation time by 60%.
Read the full case study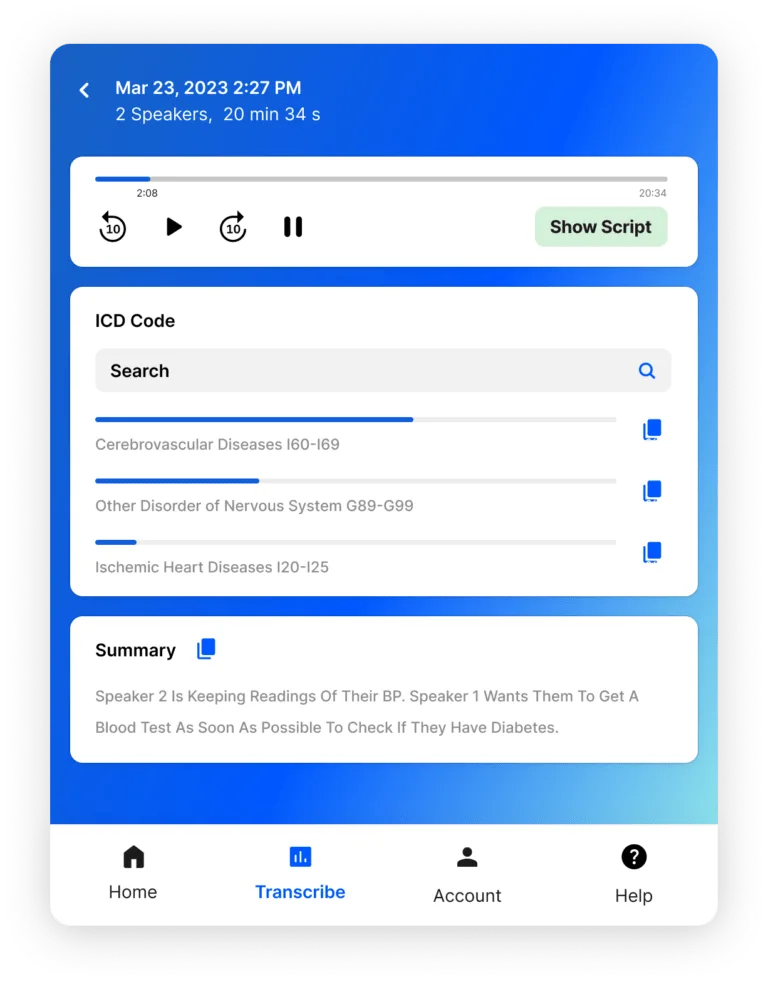
Ready to eliminate documentation burden?
Let's assess where ambient AI scribes can recover clinician time and expand your capacity.
Or call: 404.654.3855


