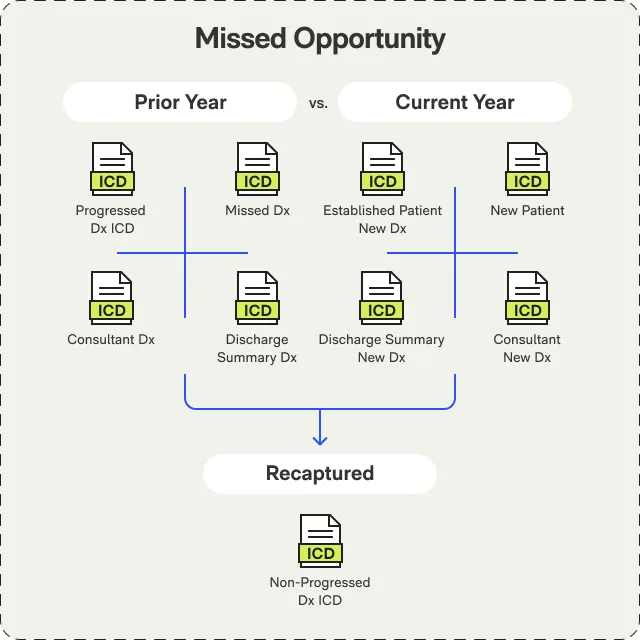
MDS Optimization & PDPM Revenue Capture
$10M in PDPM revenue recovered. $2M in quality incentives. AI-powered MDS optimization that surfaces missed diagnoses, recommends assessment timing, and fits your coordinators' existing workflow.
PDPM Revenue
Quality Incentives
Time Savings
Diagnosis Accuracy
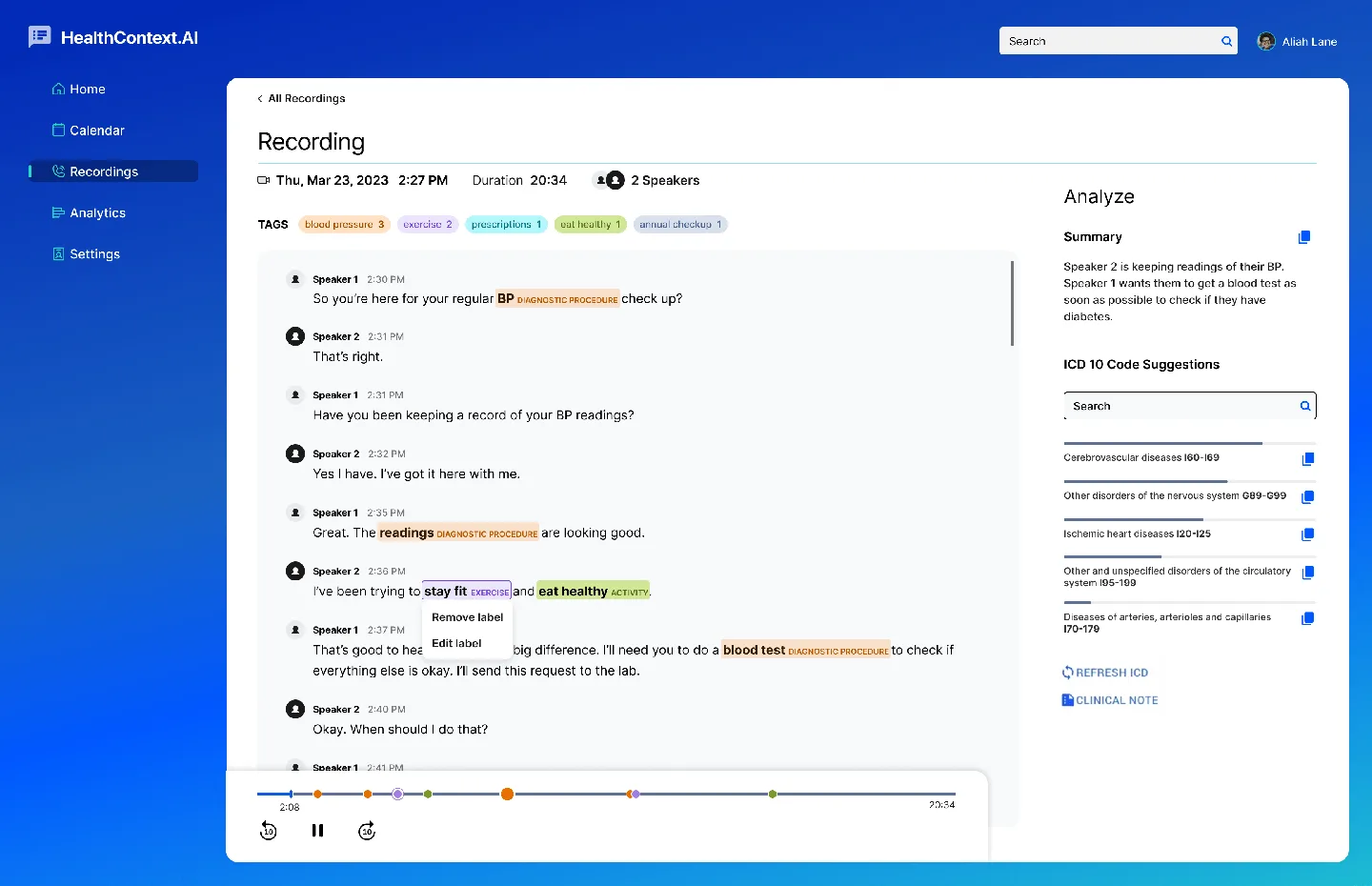
AI-powered MDS assessment optimization
MDS drives your reimbursement. PDPM determines your revenue.
The Minimum Data Set (MDS) is the comprehensive assessment required for every SNF resident. It captures clinical information, functional status, and diagnoses that directly determine your reimbursement under the Patient-Driven Payment Model (PDPM).
PDPM replaced the old RUG system in 2019, fundamentally changing how SNFs get paid. Instead of therapy minutes, payment now depends on patient characteristics-diagnoses, functional status, cognitive impairment, and clinical complexity. This means accurate MDS assessments directly impact your bottom line.
Every missed diagnosis, every incomplete assessment, every timing gap costs you money. And with CMS's focus on quality measures, MDS accuracy now affects your Five-Star rating too.
How PDPM Payment Works
Physical Therapy: Based on functional score and clinical category
Occupational Therapy: Based on functional score and clinical category
Speech-Language Pathology: Based on cognitive impairment and swallowing disorders
Non-Therapy Ancillary: Based on extensive conditions and medications
Nursing Component: Based on clinical classification and ADL score
Each component is determined by MDS data. Incomplete assessments = lower payments.
MDS coordinators are overwhelmed. Revenue is walking out the door.
Per MDS Assessment
Chart review, resident observation, family interviews, documentation-each assessment is a multi-hour process that pulls coordinators from other critical tasks.
Missed Diagnoses
Hidden in clinical notes, lab results, and medication lists. Every missed diagnosis is money left on the table-and potentially a care planning gap.
Per Day CMI Impact
A single missed comorbidity or incorrect clinical category can reduce your daily rate by over $120. Multiply by census and length of stay-the numbers add up fast.
Why Traditional Approaches Fall Short
Manual Review
Even experienced MDS coordinators can't catch every diagnosis buried in 6 months of clinical notes. They're doing their best with overwhelming data volume.
Basic EHR Alerts
PointClickCare's built-in tools are helpful but generic. They don't learn your documentation patterns or understand your specific payer requirements.
Consulting Reviews
Quarterly audits catch errors after the fact. By then, you've already submitted and been paid incorrectly. Retrospective fixes don't recover all the revenue.
Additional Staff
Hiring more MDS coordinators doesn't solve the underlying problem-they face the same data overload. And qualified coordinators are increasingly hard to find.
AI that surfaces diagnoses, recommends assessments, and fits your workflow.
We built our MDS optimization platform by spending 40+ hours shadowing MDS coordinators-watching them work, understanding their challenges, learning their workflows. The result is AI that actually helps, not another tool that creates work.
Diagnosis Discovery
Our AI continuously monitors clinical documentation, lab results, medication lists, and progress notes to identify diagnoses that should appear on the MDS. It surfaces findings with direct links to supporting documentation-so coordinators can verify quickly instead of hunting through charts.
Example: Patient on Metformin with elevated A1C in labs but no diabetes diagnosis coded. AI flags for review with supporting documentation linked.
Assessment Recommendations
Beyond just finding diagnoses, our system recommends optimal assessment timing, clinical categories, and documentation improvements. Every recommendation links to the source documentation and explains the reimbursement impact.
Example: "Consider Significant Change assessment-functional status decline documented across 3 therapy notes this week. Estimated CMI impact: +$85/day."
Pre-Submission Validation
Before you transmit, our system validates each MDS against CMS requirements and internal quality standards. It flags errors, inconsistencies, and missed opportunities-catching problems before they become audit findings or revenue losses.
Example: "ADL score inconsistent with therapy documentation. Review Section GG before submission."
Quality Measure Optimization
MDS data drives your Five-Star quality measures. Our system tracks quality measure performance in real-time, identifies residents affecting your scores, and recommends documentation or care interventions to improve outcomes.
Result: CommuniCare achieved Five-Star QM Score of 60/100 and $2M in quality incentives.
$10M+ PDPM revenue at CommuniCare. Financial analyst calculated.
Not vendor estimates. Not projections. Actual revenue recovered, validated by an independent financial analyst, from production deployment across multiple states.
CommuniCare Health Services
One of the nation's largest post-acute care providers. Multiple states, hundreds of facilities. They needed MDS optimization that could scale without adding coordinator headcount.
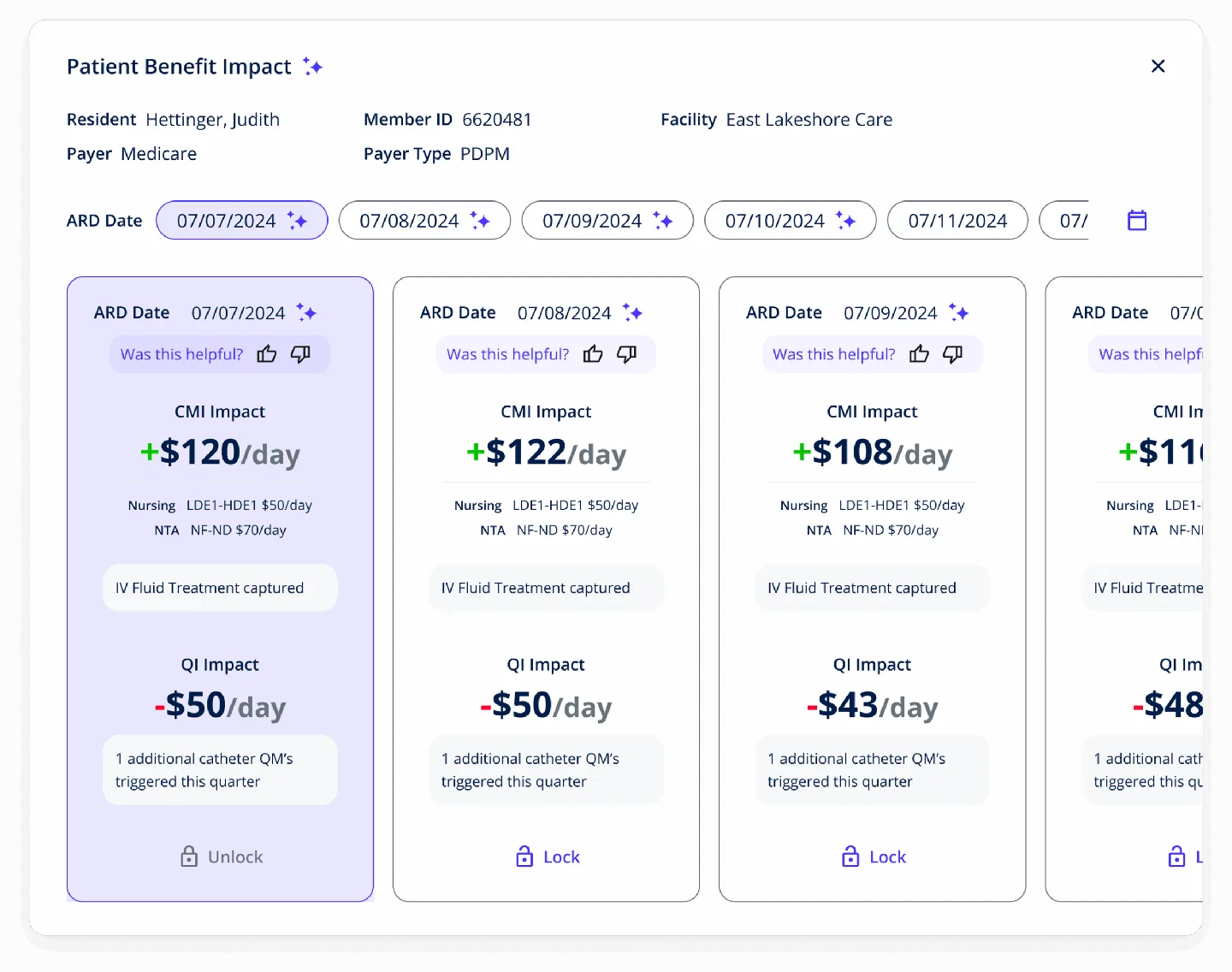
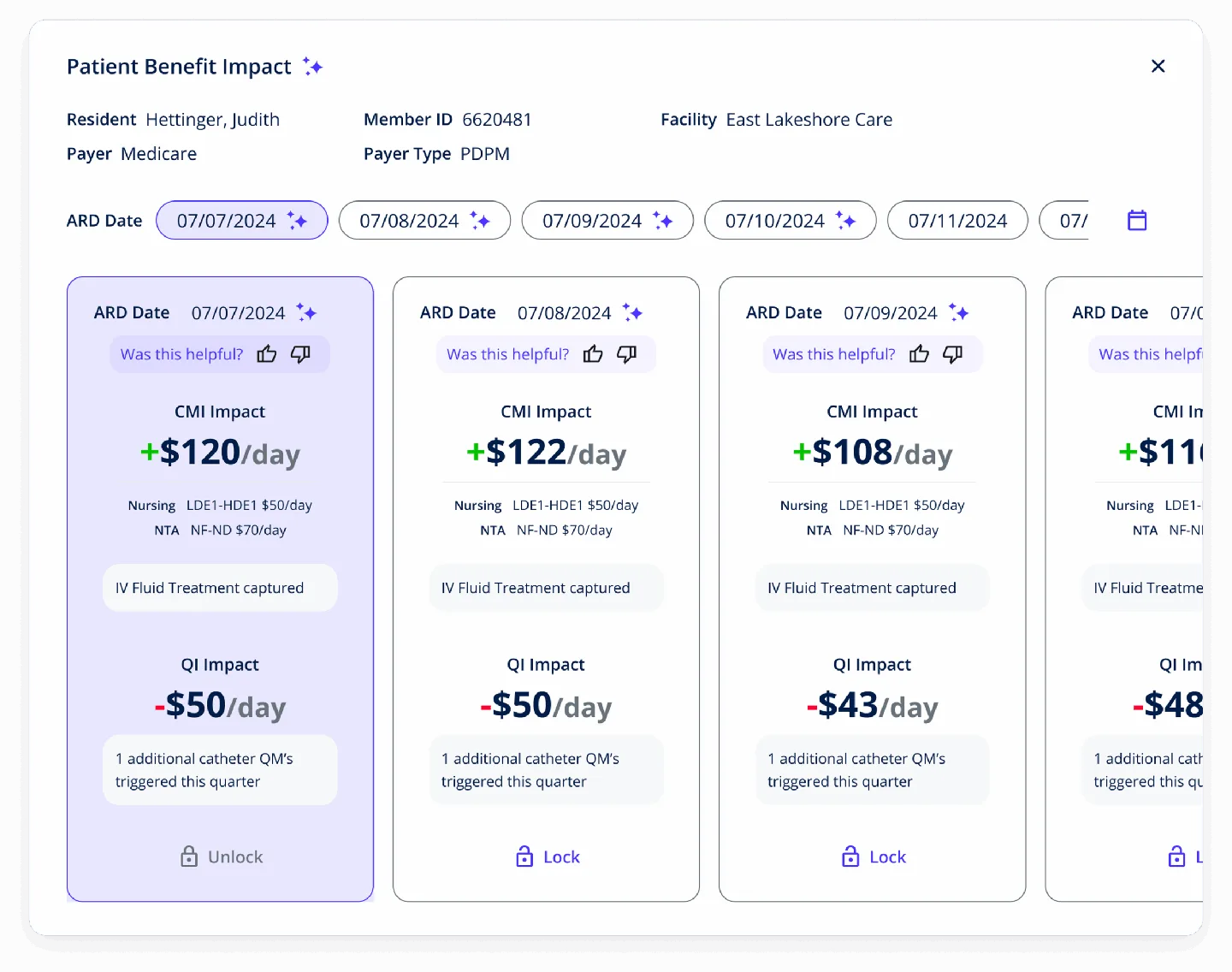
Diagnosis Capture
AI identifies 15-20% more billable diagnoses that were present in documentation but not coded on assessments.
CMI Improvement
Average Case Mix Index improvement of 0.05-0.10 through better clinical classification and complete capture.
Audit Readiness
Every AI recommendation links to source documentation-creating an audit trail that protects your revenue.
Works within PointClickCare. No separate system to manage.
Our MDS optimization integrates directly with PointClickCare-the EHR most SNFs already use. No separate login. No switching between systems. Recommendations appear where your coordinators are already working.
Integration includes bidirectional data flows: we pull clinical documentation and return recommendations. Updates happen in real-time, so coordinators always see current information.
For facilities using other EHRs, we have integration patterns for Epic, Gehrimed, and custom systems. The key is meeting your coordinators where they work.
Integration Capabilities
PointClickCare Native
Primary integration-production-proven across multiple states
Real-Time Data
Clinical notes, labs, medications-pulled as documented
Workflow Embedded
Recommendations appear within existing MDS workflow
HIPAA Compliant
Full compliance with BAAs, audit trails, access controls
How the complete value chain delivered $12M+ in results.
Most MDS optimization vendors stop at deployment. We own the complete value chain—all 10 steps, concept to scale. That's why CommuniCare achieved $10M+ in recovered revenue, not a pilot that stalled.
Discover
Data Foundation — EHR data extraction, clinical documentation mapping, baseline revenue metrics
Solution Design — 40+ hours on-site with MDS coordinators, mapped workflows and pain points
Experiment
Hypothesis & Scope — Defined AI diagnosis engine approach with explainability requirements
Build & Validate — Working software tested on real patient data with coordinator feedback
Engineer
Agile Development — Iterative sprints with continuous coordinator feedback
Systems Integration — Native PointClickCare integration, bidirectional data flows, no separate login
Change Management — Facility-level training and coordinator adoption
Production Deploy — Phased rollout across states with monitoring
Optimize
KPI Accountability — Revenue impact validated by independent financial analyst
Continuous Improvement — Ongoing model refinement, gated learning, quality measure optimization
MDS optimization is one piece of the revenue cycle puzzle.
The same methodology that recovered $10M+ in PDPM revenue powers our broader revenue cycle AI work—from RAF/HCC coding ($10M+ in risk adjustment improvements) to denial prediction, claim follow-up triage, and payer contract interpretation. If AI can find revenue hidden in clinical documentation, we've built it.
Explore Revenue Cycle AIMDS optimization often combines with these domains.
Value-Based Care
MDS data drives SNF VBP performance and ACO REACH quality measures.
Learn more →Revenue Cycle AI
PDPM revenue capture connects to broader billing and denial management.
Learn more →Documentation Automation
Better clinical documentation means better MDS assessments.
Learn more →Ambient AI Scribes
Capture clinical observations at the point of care that feed MDS accuracy.
Learn more →RAF / HCC Coding
Coordinate diagnosis capture across MDS and risk adjustment workflows.
Learn more →Frequently Asked Questions
Common questions about MDS optimization and PDPM revenue capture for skilled nursing facilities.
AI frameworks that power this domain.
Ready to recover your PDPM revenue?
30-minute call. We'll assess your MDS optimization opportunity and share what we've learned from $10M+ in recovered revenue.
Assess Your PDPM OpportunityOr call: 404.654.3855
Related Insights
From Our Blog

Healthcare Revenue Optimization: How AI Helped a Post-Acute Care Provider Generate $12M+
Mar 03, 2025

Designing With Gratitude: What Working With Nurses Taught Us About Building Human-Centered AI
Dec 03, 2025

7 Technologies Fueling the Future of Healthcare Revenue Cycle Management
Sep 09, 2025