We've already built the AI that makes VBC profitable.
The shift from fee-for-service to value-based care requires technology that most organizations don't have — and can't buy off the shelf. Risk adjustment AI, MDS optimization, virtual care platforms, revenue cycle intelligence. Not as separate tools. As an integrated technology stack.
We've built all of it. In production. Across 7 states. With $20M+ in verified financial impact.
Assess Your VBC Technology Needs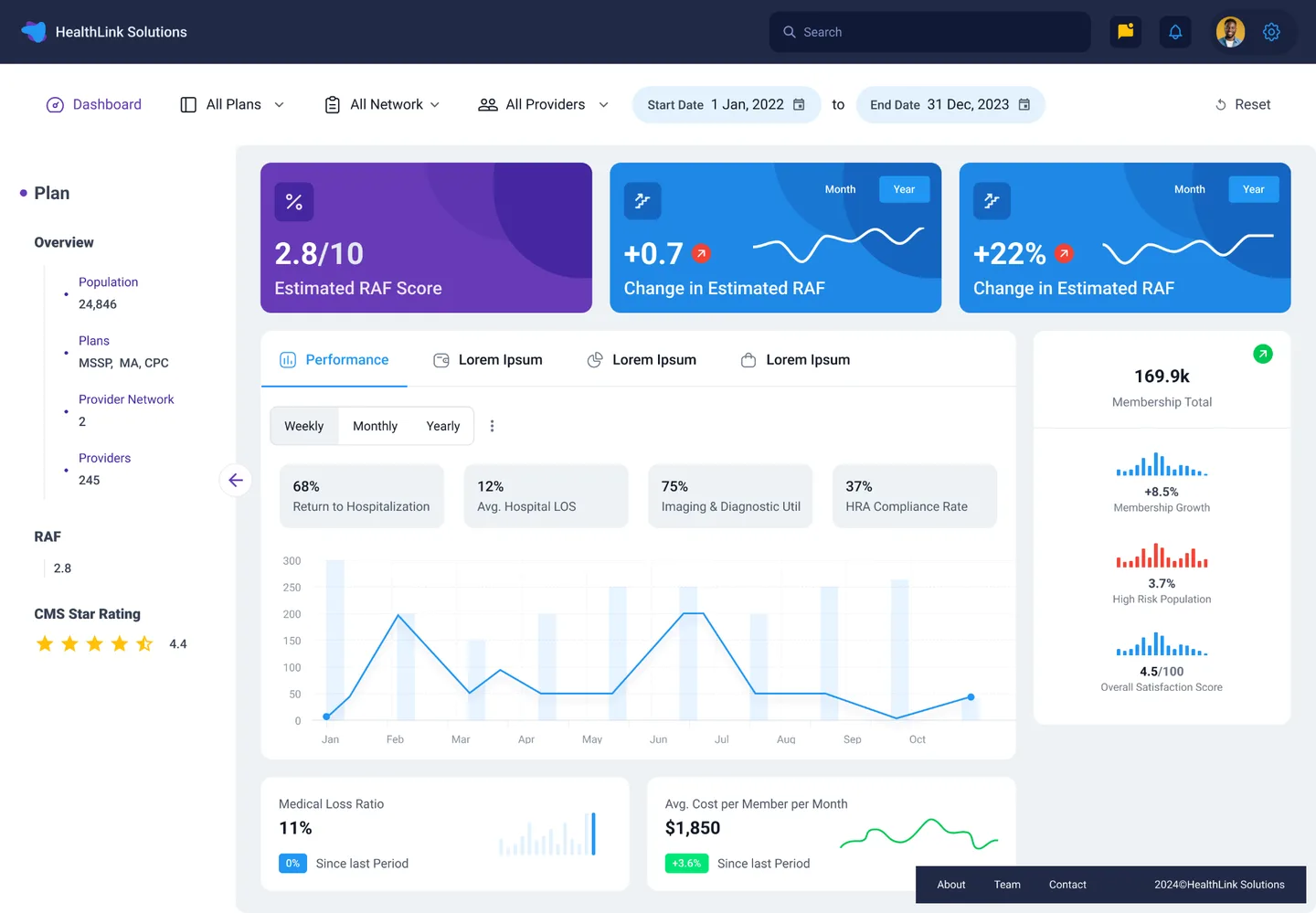
VBC Accelerator Prototype — Population Health Dashboard
Verified Financial Impact
Patients Managed
Treat-in-Place Rate
Diagnosis Accuracy






Fee-for-service is ending. The technology gap is the real risk.
CMS is accelerating the transition to value-based care. By 2030, every Medicare beneficiary will be in a value-based arrangement. Organizations without the technology to manage risk, track quality, coordinate care, and optimize reimbursement won't survive the shift.
VBC requires a fundamentally different mindset: managing populations instead of individual encounters. Incorporating payer logic into provider workflows. Thinking about total cost of care, not just per-visit revenue. This isn't a billing change — it's an operating system change.
Most EHRs weren't designed for this. They capture clinical data but don't surface the analytics needed to manage populations, predict risk, or optimize quality scores. Custom AI bridges this gap — and we've built it at scale.
VBC Programs We Support
SNF VBP (Skilled Nursing Facility Value-Based Purchasing)
Readmission reduction, quality measure optimization, incentive payment maximization.
ACO REACH
Risk adjustment, care coordination, quality reporting, shared savings optimization.
MSSP (Medicare Shared Savings Program)
Population health management, quality measure performance, cost benchmarking.
Medicare Advantage (MA-SNP, D-SNP)
RAF optimization, HEDIS measures, Star Ratings performance.
From the deck:
"Utilize advanced analytics and AI to improve diagnosis accuracy, population risk scores and reimbursement rates — at the Plan, Network, and Provider level."
Five production AI solutions. One integrated VBC technology stack.
Each solution addresses a critical component of value-based care success. Together, they form the technology foundation that VBC organizations need to manage populations, optimize reimbursement, and demonstrate quality.
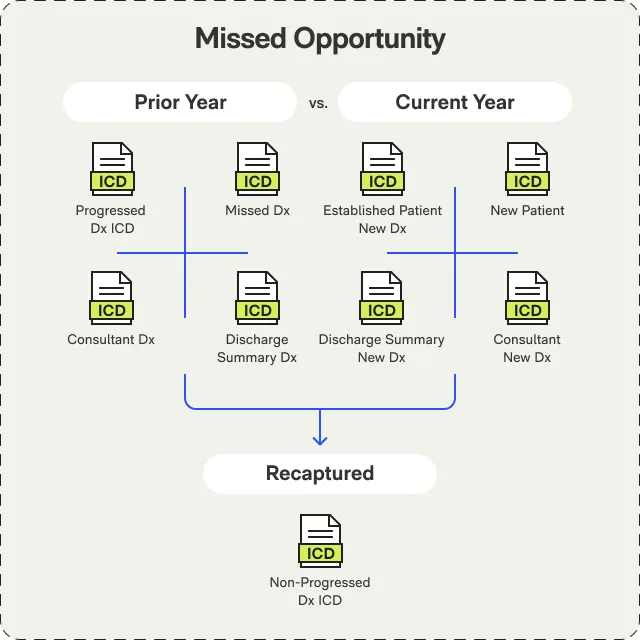
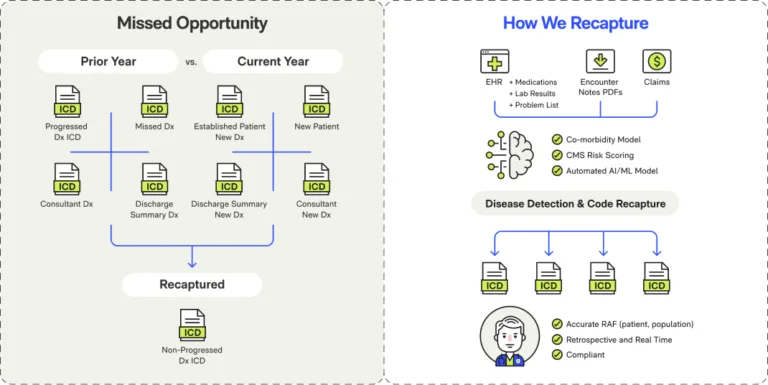
Medical Coding AI
AI that reviews patients 50X faster than manual audit with 90%+ accuracy. Surfaces missed HCC codes from 6 clinical data sources with audit-defensible evidence chains.
RAF Improvements
Diagnosis Accuracy
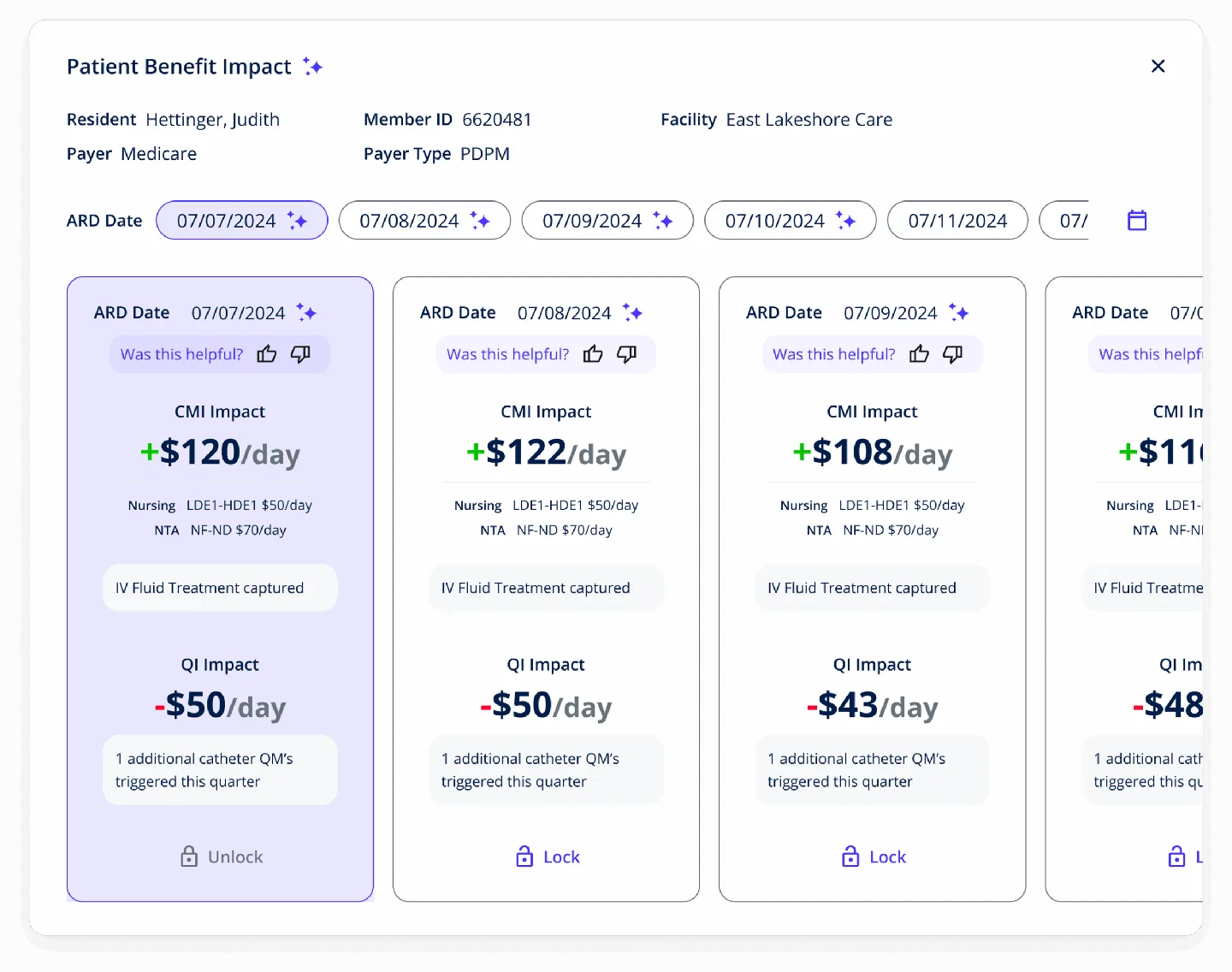
MDS Optimization
AI-powered MDS assistant built after 40+ hours shadowing coordinators. Surfaces missed diagnoses, validates assessments pre-submission, and optimizes quality measures.
PDPM Revenue
Quality Incentives

NeverAlone Platform
24/7 virtual care platform we built and operate in production. Treatment-in-place reduces costly hospital transfers — the single biggest cost driver in VBC models.
Patients Served
Treat-in-Place
Revenue Cycle Intelligence
AI agents for A/R prioritization, denial prediction, contract interpretation, and intelligent appeals. Trained on your payer contracts and historical patterns.
Days in A/R
Denial Rate

Population Health Analytics & Benchmarking
The analytical backbone of VBC. Population-at-a-glance dashboards, patient-level impact analysis, provider benchmarking, cost trend forecasting, and real-time KPI tracking — all from a centralized patient data platform that links records across systems.
Audit Reporting
Quality Measures
RAF Transition
Risk adjustment forecasting, MDS reporting, population health benchmarking, claims analysis, HRA audit reporting, and model of care review.
Not projections. Production results from real VBC programs.
Every number below comes from systems we built and operate. Financial analyst-calculated, not vendor estimates.
Total Verified Impact
Patients Managed
Treat-in-Place Rate
Diagnosis Accuracy
Facilities Live
Providers on Platform
Changing the conversation at the point of encounter.
VBC success starts at the point of care. We build a centralized patient data platform that compresses a lifetime of health encounters and surfaces actionable insights to providers in their EHR — at the moment they need them.
Point of Encounter
Centralized patient data center — linking clinical encounters, claims, medications, and population health data
Population Health
Risk stratification, care gap identification, panel management
Quality of Care
HEDIS, Star Ratings, quality measure optimization
Risk Management
RAF optimization, shared savings, cost benchmarking
Staffing Efficiency
AI-assisted workflows, 50X review speed, reduced admin burden
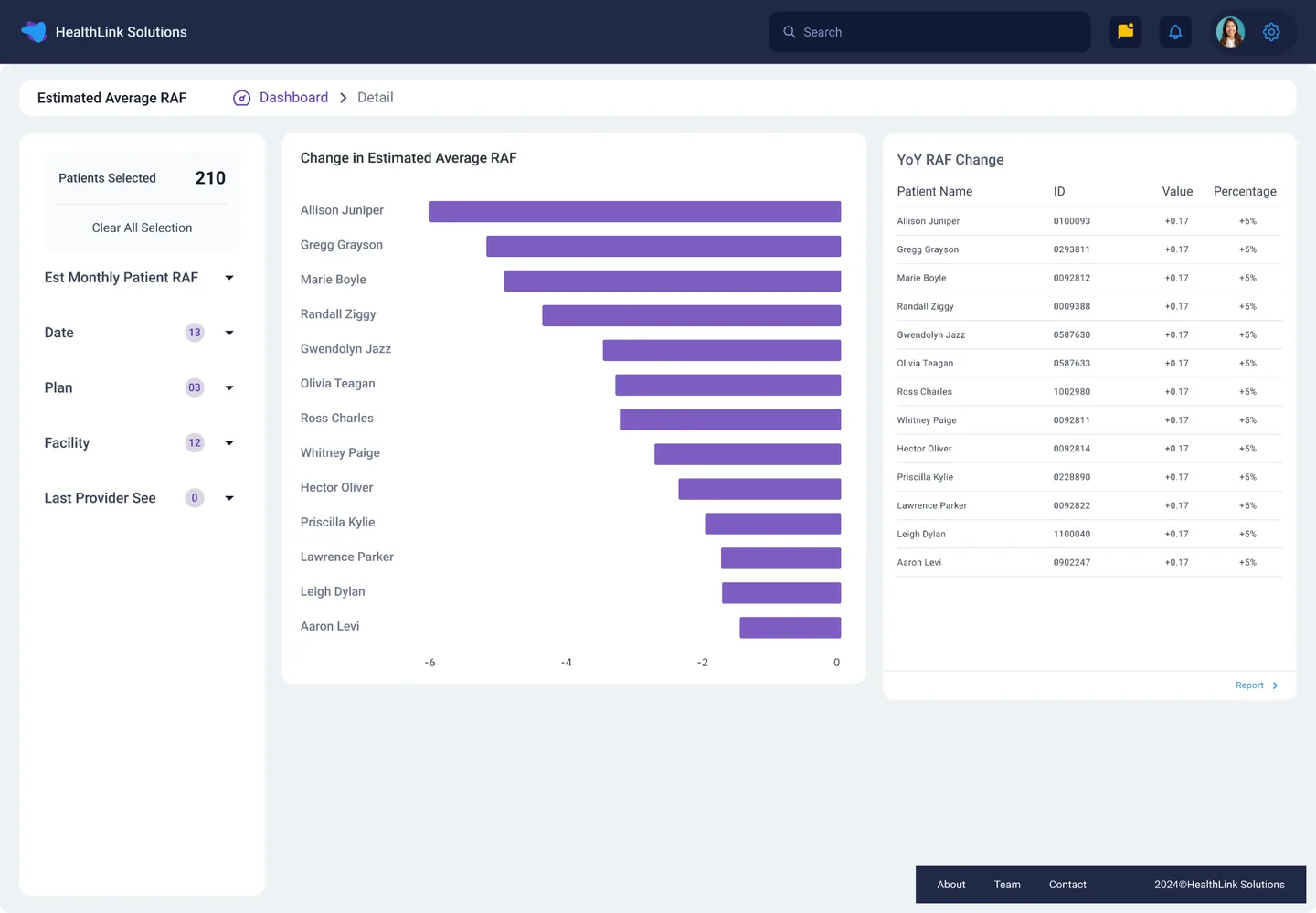
Plan Level Intelligence
Patient-level RAF tracking, YoY diagnosis comparison, portfolio risk scoring, and shared savings projections.
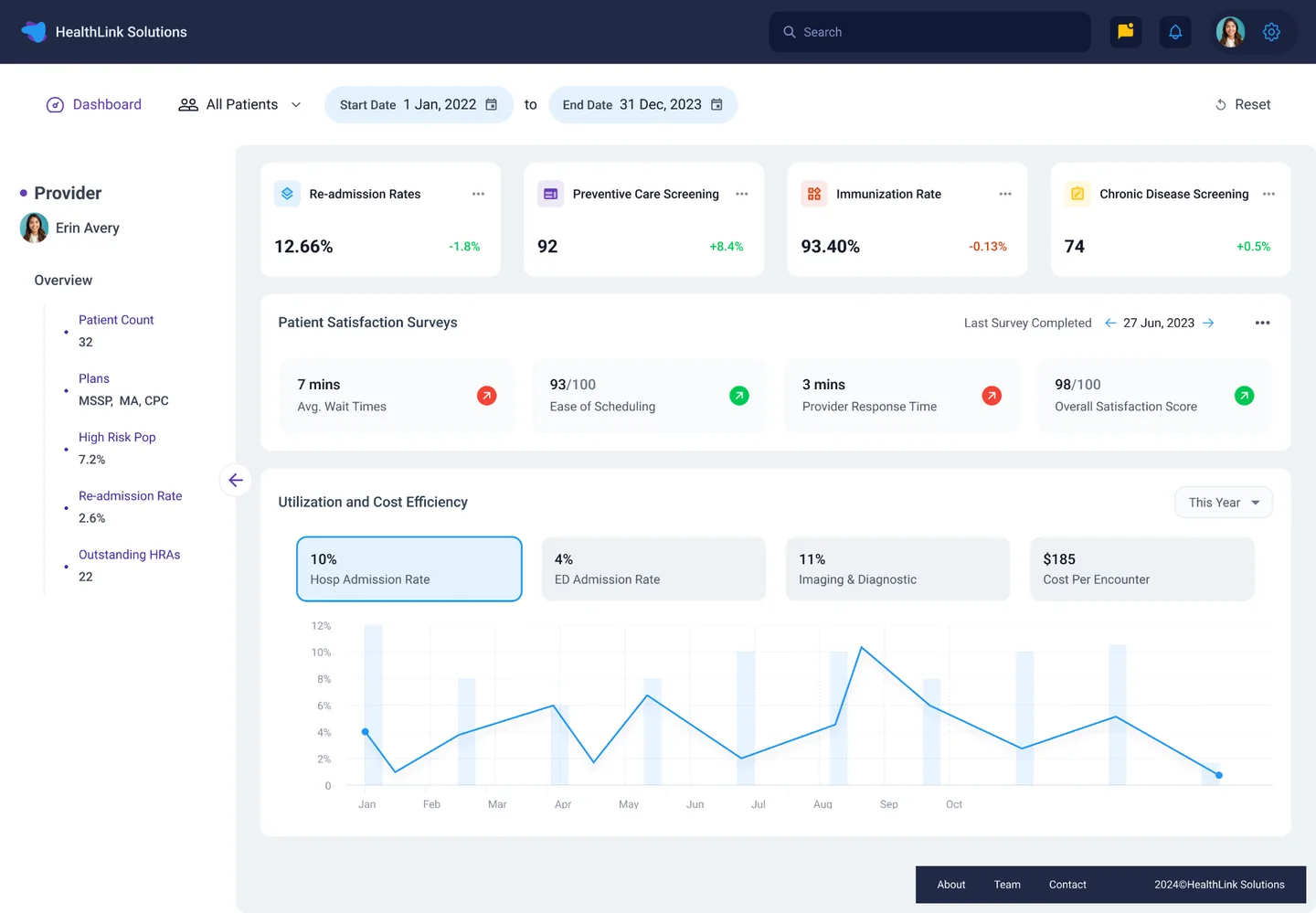
Provider Level Intelligence
Readmission rates, screening metrics, patient satisfaction, utilization and cost efficiency by provider.
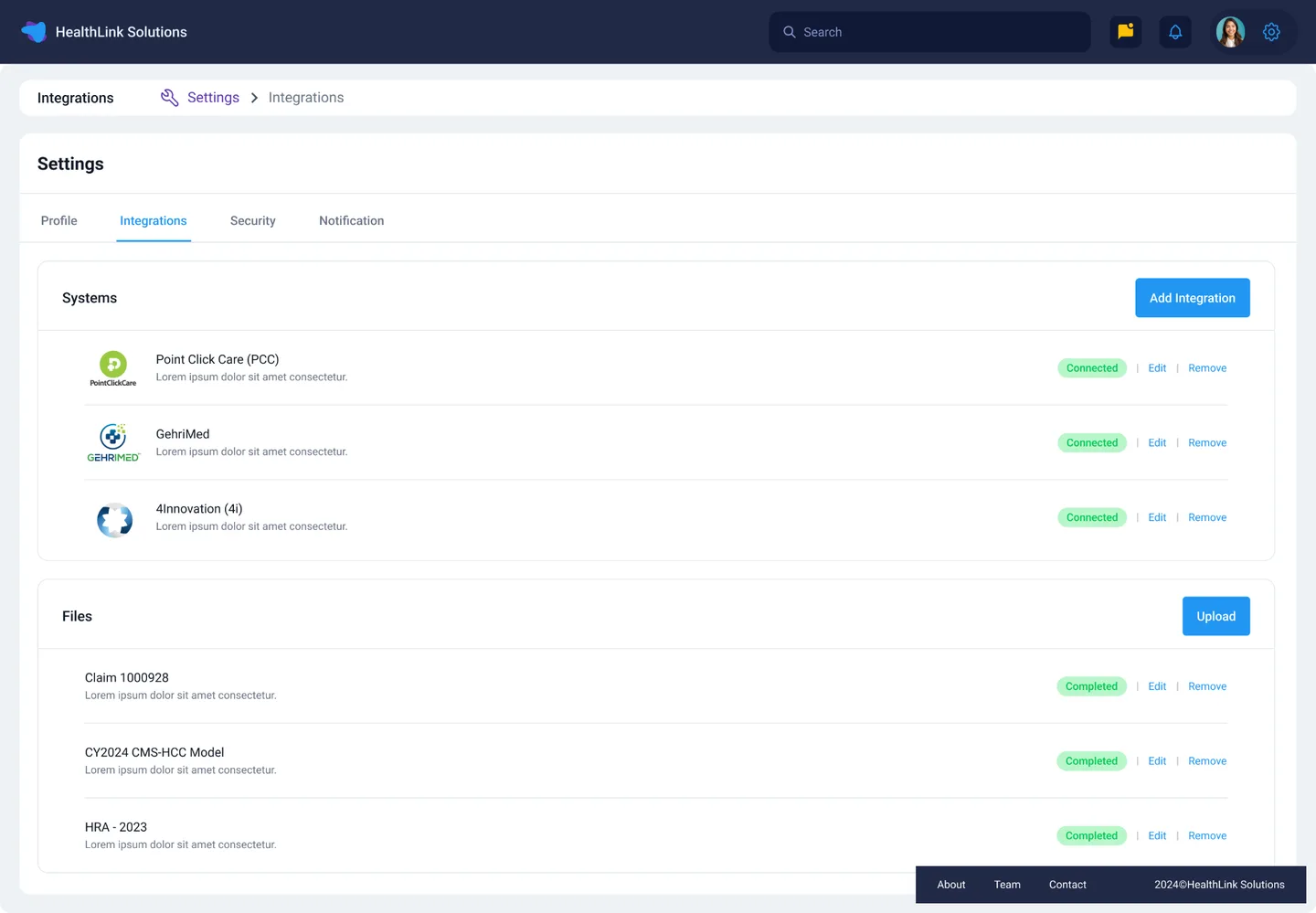
Data Interoperability
Standardized EHR integrations, claims file uploads, and cross-platform patient data linking.
VBC Accelerator — explore the product.
We didn't just talk about building a VBC analytics platform. We designed it. Click through the interactive prototype to see population health dashboards, patient-level RAF analysis, provider benchmarking, and EHR integrations — built for ACO REACH and Medicare Advantage plans.
Click through the prototype to explore dashboards, patient analysis, provider benchmarking, and integrations.
We're not a vendor. We're an operator.
Most VBC technology vendors sell you software. We build, deploy, and operate the systems ourselves — then transfer when you're ready. That's why everything we build reaches production.
Typical VBC Technology Vendors
One-size-fits-all platforms
Same dashboards for SNF VBP, ACO REACH, and MA plans
Sell and disappear
License software, provide training, call it done
Generic analytics
Reports that don't change behavior at the point of care
No skin in the game
Revenue tied to licenses, not your outcomes
The DS VBC Partnership
Custom AI for your specific programs
Built for your VBC contracts, your patient population, your quality targets
We operate what we build
26K patients on NeverAlone. We run it 24/7, not just build it.
Intelligence at the point of care
Insights delivered in EHR workflows — not dashboards nobody checks
Outcomes-tied engagement
$20M+ verified impact. Contractually tied to your KPIs.
Our complete VBC value chain:
Managing a population requires all of these working together.
VBC isn't about individual tools. It's about an integrated technology stack where risk adjustment informs care coordination, virtual care reduces readmissions, quality data drives reimbursement, and revenue cycle optimization captures everything you've earned.
Identify Risk
Medical Coding AI + MDS Optimization
Accurate risk adjustment captures the true complexity of your population. RAF/HCC AI identifies missed diagnoses. MDS optimization ensures every assessment drives appropriate reimbursement. Together: $20M+ in recovered revenue.
Reduce Utilization
NeverAlone Virtual Care
Hospital transfers are the single biggest cost in VBC. NeverAlone delivers 96% treatment-in-place by connecting care teams to providers in real-time, 24/7. Across 130+ facilities and 7 states in production.
Demonstrate Quality
Population Health Analytics
Quality scores drive incentive payments and determine shared savings eligibility. Our analytics track HEDIS, Star Ratings, and program-specific quality measures in real time — not after the year ends.
Capture Revenue
Revenue Cycle Intelligence
Even with perfect clinical outcomes, revenue leaks through denials, underpayments, and slow A/R. Revenue Cycle AI automates the financial operations side of VBC — from claim submission to appeal generation.
Standardized integrations. Your data, unified.
VBC requires linking patient data across platforms. Our data engineering framework connects EHRs, claims, labs, and quality registries into a single patient record — enabling the analytics that VBC demands.
EHR Systems
Production integrations with PointClickCare, Epic, Gehrimed, Elation, and Acclivity.
Bidirectional, real-time
Claims Data
Medicare, Medicaid, and commercial payer claims for utilization analysis and cost trending.
Historical + real-time
HIE / ADT Feeds
Real-time admission, discharge, and transfer notifications for care coordination.
Event-driven alerts
Quality & Compliance
CMS quality programs, registry reporting, HEDIS submission, and audit documentation.
Automated reporting
Data engineering capabilities:
VBC expertise built on deep domain knowledge.
RAF / HCC Coding
Risk adjustment AI powering VBC reimbursement accuracy.
$10M+ →
MDS / PDPM Optimization
AI-powered MDS assessments driving PDPM revenue and quality.
$12M+ →
Revenue Cycle AI
AI agents for every stage of the financial operations pipeline.
200-300 bps →
EHR Integrations
Production integrations with 5+ EHR platforms.
Learn more →
Ambient AI Scribes
Clinical documentation that feeds quality measures and risk capture.
80% time saved →
Ready to make your VBC transition profitable?
Let's assess your value-based care technology needs and show you how production AI can accelerate your transition from fee-for-service to value-based care.
Or call: 404.654.3855
Related Insights
From Our Blog

Leveraging AI tools in Social Need Screening and Intervention – comments on proposed changes to HEDIS SNS-E measure
Feb 19, 2025

AI & The Job Landscape, ChatGPT’s Role, & The Future of RPM
Dec 12, 2023

Confronting the Challenges and Opportunities of AI in Healthcare
Dec 12, 2023