Revenue Cycle AI
Your revenue cycle is drowning in manual processes. 45-day A/R cycles. 12% denial rates. Staff chasing the same problems over and over. AI agents can transform this-but only if they're built for healthcare's complexity.
Days in A/R
Denial Rate
bps EBITDA
Admin Cost Reduction
AI agents that understand healthcare reimbursement
Revenue cycle management touches every financial transaction in healthcare-from patient registration through final payment collection. It's also one of the most complex operational areas, with thousands of payer rules, constantly changing regulations, and high-stakes decisions made under time pressure.
Generic automation tools can handle simple tasks, but healthcare revenue cycle requires AI that understands the nuances: why certain claims get denied, which accounts are actually collectible, how to interpret contract terms, and when to escalate to human review.
We build AI agents that work alongside your revenue cycle team-not as black boxes, but as intelligent assistants that explain their reasoning and learn from your specific payer mix, patient population, and operational patterns.
Why Revenue Cycle Is Hard for Generic AI
Payer Complexity
Thousands of payer-specific rules, contract terms, and submission requirements that change frequently.
Regulatory Environment
CMS updates, state Medicaid rules, commercial payer policies-the landscape shifts constantly.
Clinical Documentation
Coding accuracy depends on clinical documentation quality-revenue cycle AI must understand clinical context.
Appeal Strategy
Knowing when and how to appeal requires pattern recognition across thousands of past decisions.
Manual processes are bleeding margin
Most healthcare organizations leave significant revenue on the table through inefficient revenue cycle operations.
Average Days in A/R
Cash sitting in receivables instead of funding operations. Industry leaders achieve 28 days or better.
Initial Denial Rate
Many denials are preventable with better pre-submission edits and documentation.
Admin Overhead
Back-office costs consuming margin that should be flowing to patient care.
AI agents for every stage of the revenue cycle
We build intelligent agents that handle the cognitive work of revenue cycle management-trained on your specific workflows, payer contracts, and historical patterns.
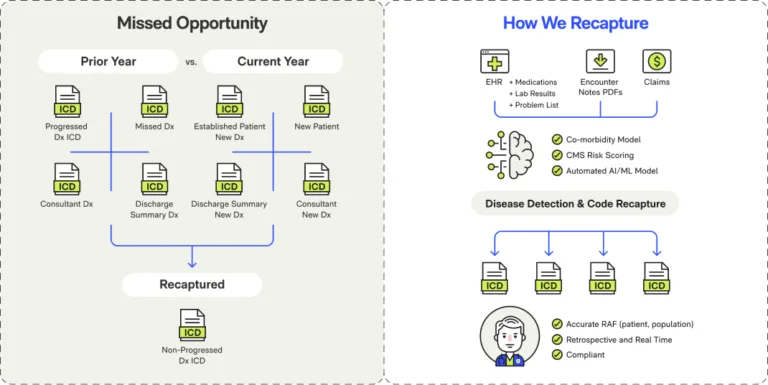
A/R Prioritization & Work Queues
Not all receivables deserve equal attention. AI-powered collectability scoring prioritizes accounts by likelihood of payment, time sensitivity, and effort required. Your team focuses on accounts that will actually pay.
Denial Prediction & Prevention
Identify claims likely to be denied before submission. The AI learns from your denial history to flag potential issues-missing documentation, coding inconsistencies, authorization gaps-so problems are fixed before they cost you money.
Contract Interpretation
Payer contracts are complex documents with buried terms that affect reimbursement. AI agents parse contract language, identify relevant provisions, and flag discrepancies between expected and actual payment.
Intelligent Appeals
When claims are denied, AI generates appeal letters tailored to the specific denial reason and payer, citing relevant contract terms and clinical documentation. Automate the routine, escalate the complex.
Coding Assistance
AI reviews clinical documentation and suggests appropriate codes, flags potential compliance issues, and identifies opportunities to capture accurate reimbursement. Human coders review and approve.
Patient Liability Estimation
Accurate patient responsibility estimates improve collections and patient satisfaction. AI analyzes coverage, calculates liability, and enables point-of-service collection with confidence.
Revenue cycle improvements you can measure
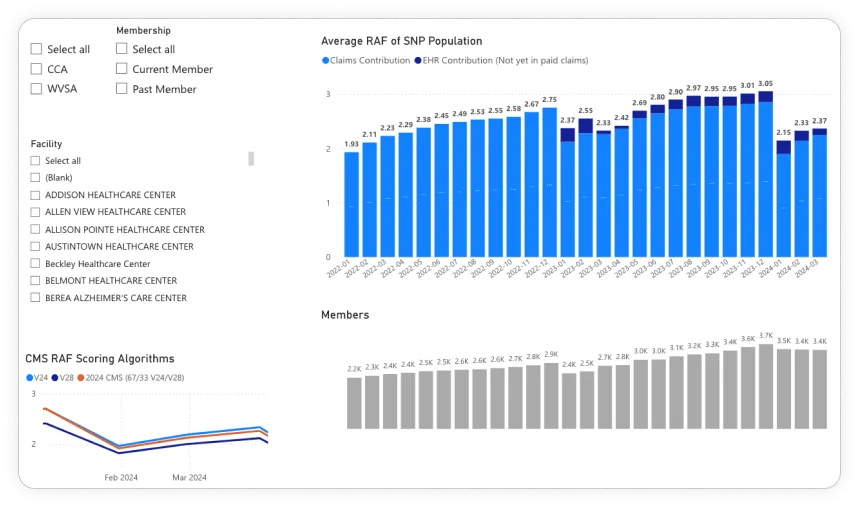
Revenue Cycle Transformation
Across our healthcare AI deployments, we consistently see revenue cycle improvements that translate directly to margin expansion.
Days in A/R
Denial Rate
bps EBITDA Improvement
Admin Cost Reduction
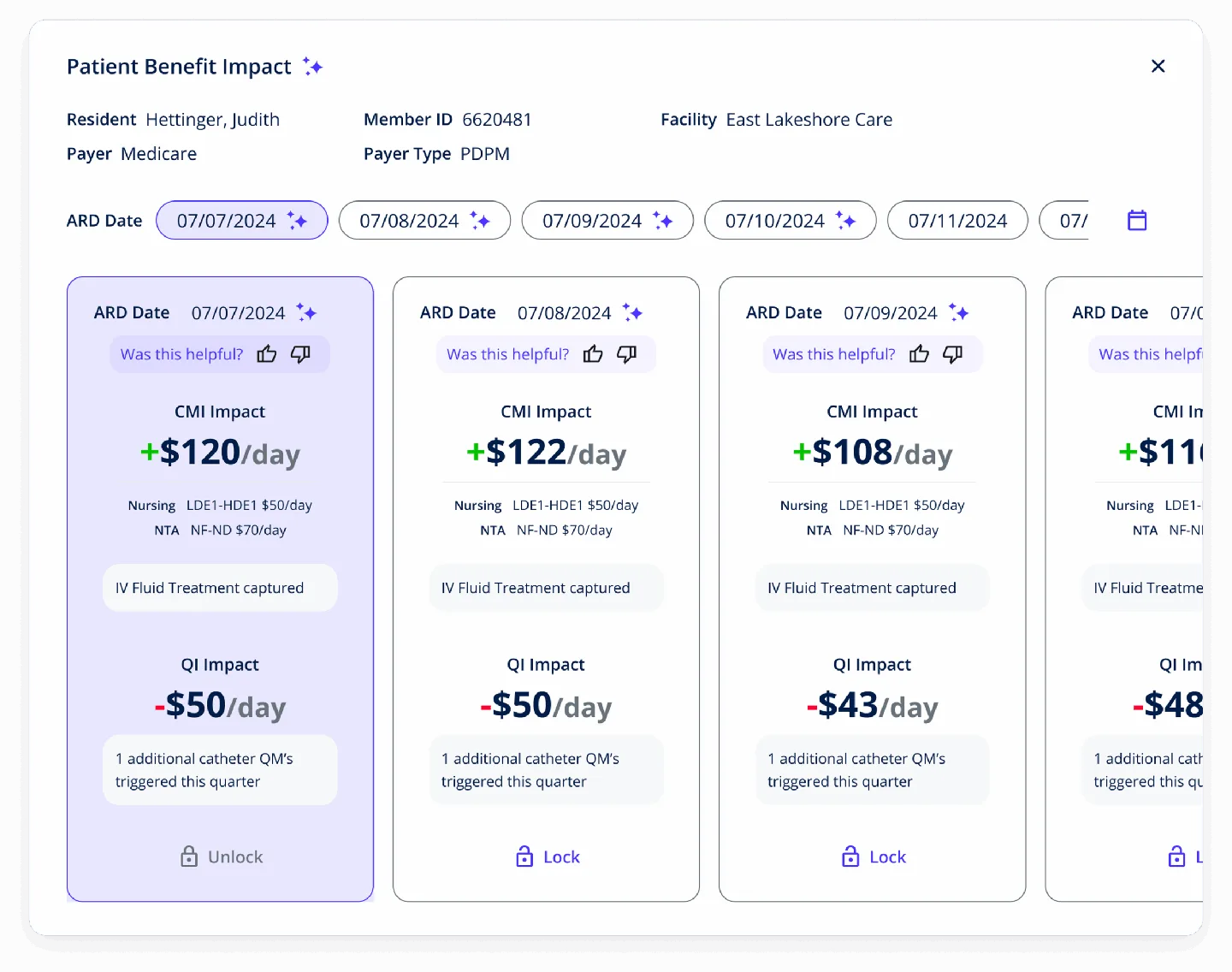
Revenue Capture Excellence
Revenue cycle optimization works best when paired with accurate clinical documentation and coding. Our MDS AI has proven impact.
PDPM Revenue Recovered
Quality Incentives
Works with your existing systems
Revenue cycle AI requires deep integration with billing systems, EHRs, and clearinghouses. We have production experience with the platforms you use.
Practice Management
Integration with PM systems for claims, patient demographics, and payment posting.
EHR Systems
PointClickCare, Epic, Gehrimed, Elation-bidirectional data flows for clinical context.
Clearinghouses
Integration with clearinghouses for claims submission, status tracking, and ERA processing.
Payer Portals
Automated eligibility checks, prior auth status, and claims inquiry where available.
Often combined with
MDS / PDPM Optimization
Accurate MDS assessments drive PDPM reimbursement upstream.
Learn more →RAF / HCC Coding
Risk adjustment accuracy directly impacts revenue for VBC organizations.
Learn more →Intelligent Back-Office Agents
Revenue cycle AI is part of our broader back-office automation framework.
See framework →Ambient AI Scribes
Complete documentation at the point of care means cleaner claims downstream.
Learn more →EHR Integrations
Revenue cycle automation requires deep integration with clinical and billing systems.
Learn more →Frequently Asked Questions
Common questions about AI-powered revenue cycle management for healthcare organizations.
AI frameworks that power this domain.
Ready to transform your revenue cycle?
Let's assess where AI can deliver the fastest ROI in your revenue cycle operations.
Or call: 404.654.3855
Related Insights
From Our Blog

Leveraging AI tools in Social Need Screening and Intervention – comments on proposed changes to HEDIS SNS-E measure
Feb 19, 2025

AI & The Job Landscape, ChatGPT’s Role, & The Future of RPM
Dec 12, 2023
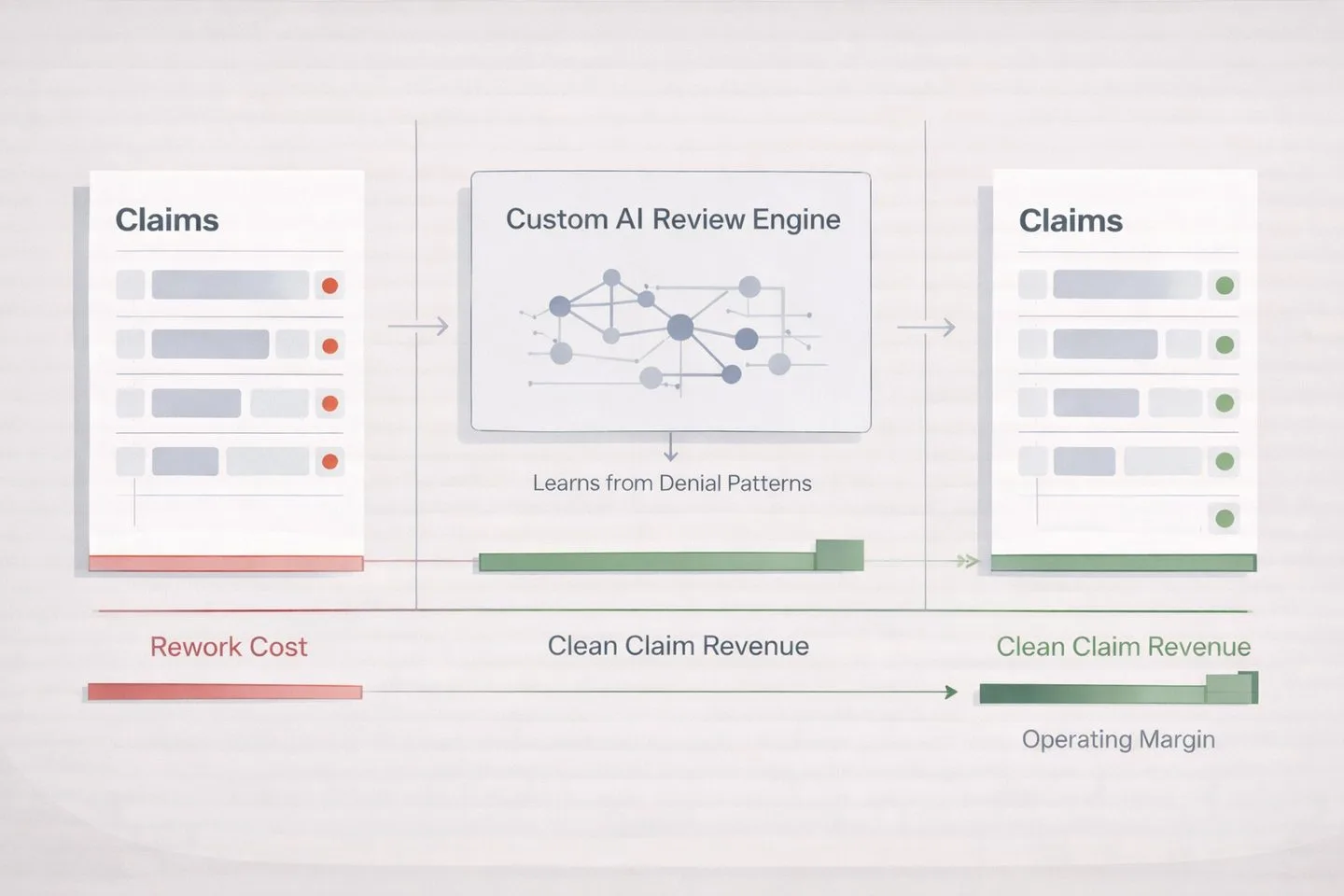
Leveraging AI for ROI in Healthcare: 10 Custom Solutions for 2026
Nov 28, 2025