RAF & HCC Coding AI
$10M+ in risk adjustment improvements. 90%+ diagnosis accuracy. 20,000+ patients across 7 states with 245 providers.
Risk adjustment determines how you get paid in Medicare Advantage, ACO REACH, and value-based contracts. Accurate HCC coding isn't just about revenue-it's about getting reimbursed appropriately for the patients you actually serve.
Assess Your RAF OpportunityRisk Adjustment Improvements
Diagnosis Accuracy
Patients Served
States in Production
Your RAF score determines your payment. HCC coding determines your RAF.
The Risk Adjustment Factor (RAF) is CMS's way of adjusting payments based on how sick your patients are. Sicker patients with more chronic conditions get higher RAF scores, which means higher payments to cover their expected costs.
Hierarchical Condition Categories (HCCs) are the diagnosis groupings that drive your RAF score. Each HCC has a specific coefficient-conditions like diabetes with complications, heart failure, and COPD add to your RAF and increase your payment.
The key: HCCs must be documented and coded annually. A patient with diabetes last year doesn't automatically count this year-the condition must be documented in the current measurement period. That's where most organizations leave money on the table.
Why RAF Accuracy Matters
Medicare Advantage
MA plans receive capitated payments based on member RAF scores. Under-coded members mean you're paid less than required to care for them.
ACO REACH
Risk adjustment determines your benchmark. Low RAF scores mean artificially low targets-making shared savings harder to achieve.
Value-Based Contracts
Commercial payers increasingly use risk adjustment. Accurate coding ensures fair payment for the complexity you manage.
Every missed HCC is money left on the table-and inaccurate risk representation to payers.
Chronic conditions disappear from documentation. Revenue follows.
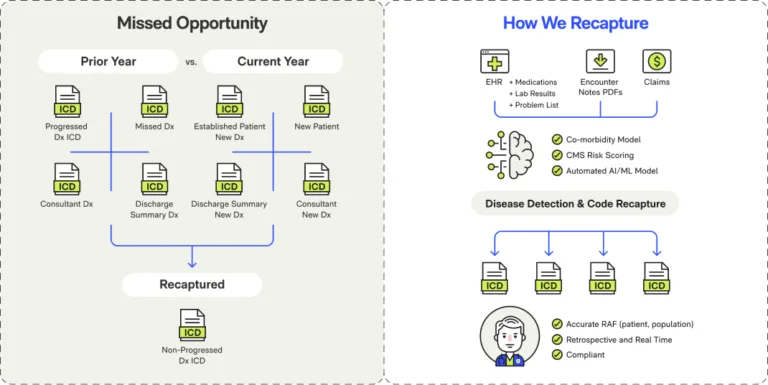
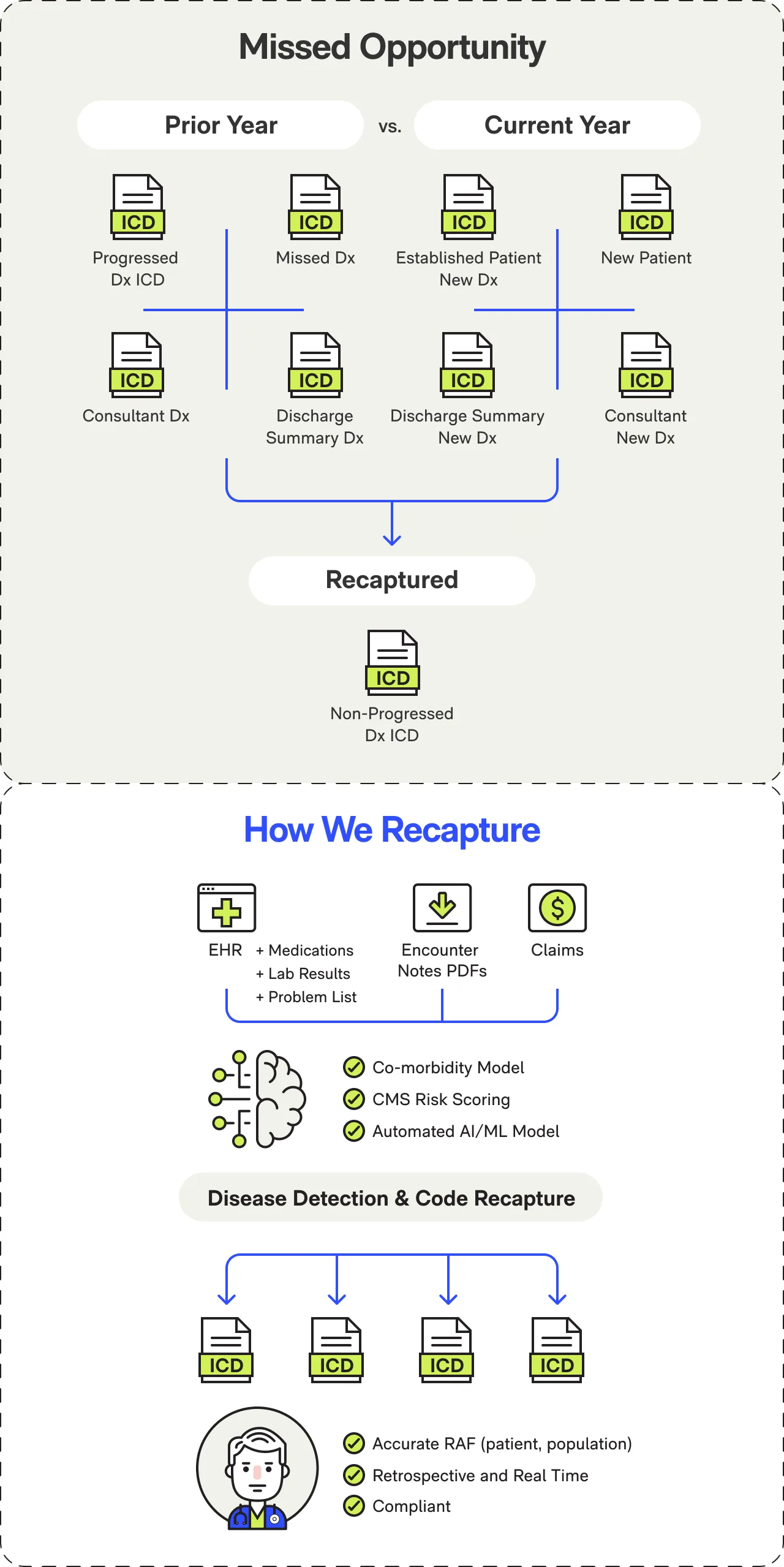
HCC Recapture Gap
Known chronic conditions documented in prior years often don't get re-documented annually. Diabetes, heart failure, COPD-conditions don't resolve, but documentation gaps make them invisible to risk adjustment.
Suspected Conditions
Clinical evidence suggests conditions that were never formally diagnosed. Medications, lab values, and symptoms point to HCCs hiding in plain sight.
Per Patient Impact
Annual revenue impact of accurate vs. incomplete RAF coding. For a 10,000-patient population, that's $50M-$150M in risk adjustment accuracy at stake.
The Documentation Challenge
Annual Recapture Requirement
HCCs must be documented every measurement year. A diabetic patient from 2024 needs 2025 documentation to count toward 2025 RAF-regardless of how chronic the condition is.
Provider Cognitive Load
Primary care physicians manage 15-25 patients daily with 10-15 chronic conditions each. Remembering which HCCs need documentation is impossible without system support.
Specificity Requirements
Generic diagnosis codes often miss HCC opportunities. "Diabetes" isn't enough-the type and complications must be specified for proper risk adjustment.
Audit Exposure
CMS audits risk adjustment accuracy. Over-coding creates compliance risk; under-coding leaves money on the table. You need accuracy, not just volume.
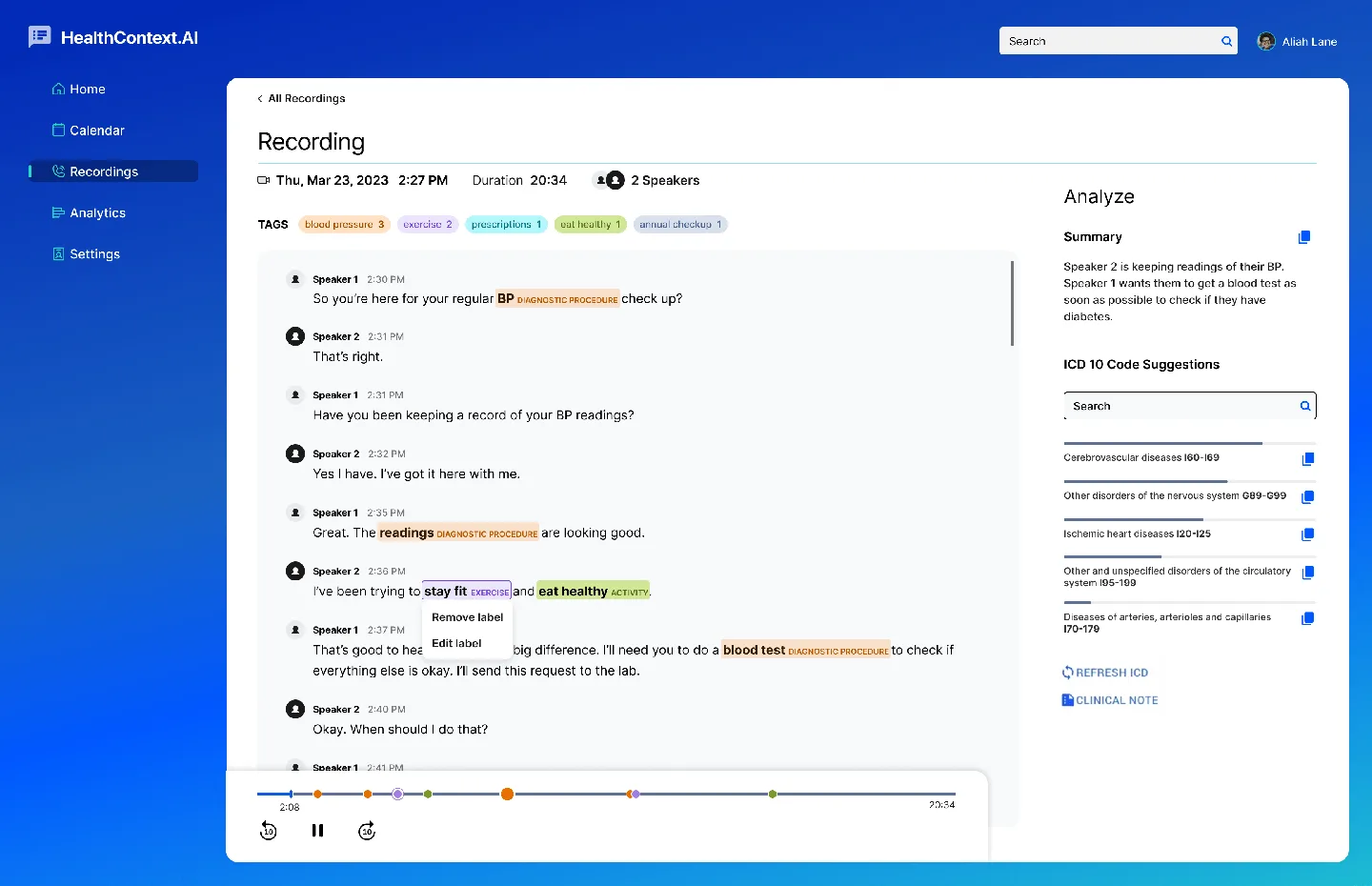
AI that identifies HCC opportunities with explainable evidence.
We built our RAF optimization platform using peer-reviewed CMS methodologies and clinical NLP. Every recommendation links to source documentation-creating audit-defensible accuracy, not black-box suggestions.
HCC Recapture
Our system continuously monitors for known HCCs from prior years that need current-year documentation. It alerts providers before visits, identifies documentation gaps, and tracks recapture status across your entire population.
Example: "Patient has HCC 18 (Diabetes with Chronic Complications) from 2024. No 2025 documentation found. Recommend addressing at upcoming visit."
Suspected Condition Identification
AI analyzes medications, lab results, and clinical notes to identify conditions that may be present but never formally diagnosed. Every suspicion includes supporting evidence for clinical review.
Example: "Patient on Metformin + Glipizide with A1C of 8.2%-no diabetes diagnosis coded. Consider HCC 19 evaluation."
Specificity Enhancement
Generic codes often miss HCC opportunities. Our system identifies where diagnosis specificity could improve risk adjustment accuracy-differentiating between types, complications, and severity levels.
Example: "E11.9 (Type 2 Diabetes without complications) coded, but neuropathy symptoms documented. Consider E11.42 for HCC 18."
Audit-Ready Documentation
Every AI recommendation links directly to supporting documentation-labs, notes, medication lists. This creates an audit trail that protects your revenue while ensuring clinical accuracy.
Result: 90%+ diagnosis accuracy with full documentation linkage for CMS audit defense.
90%+ accuracy built on peer-reviewed CMS methodologies.
Our RAF optimization isn't a black box. We use peer-reviewed CMS scoring models and clinical NLP trained on millions of healthcare documents. Every recommendation is explainable-you can see exactly why the AI flagged a condition.
This explainability matters for three reasons: clinicians trust it, auditors accept it, and you can validate accuracy before acting on recommendations.
The result: 90%+ diagnosis accuracy across 20,000+ patients, with documentation linkage that stands up to CMS scrutiny.
Under the Hood
CMS HCC Model V28: Current risk adjustment methodology with proper coefficient mapping
Clinical NLP: Trained on millions of healthcare documents for condition extraction
Multi-Source Integration: EHR, claims, labs, medications-holistic patient view
Confidence Scoring: Each recommendation includes confidence level and supporting evidence strength
Audit Trail: Complete documentation linkage for every flagged condition
$10M+ improvements across 20,000+ patients in 7 states.
Production deployment at scale. Not a pilot. Not a projection. Real results from value-based care organizations managing real patient populations.
Value-Based Care Provider
Multi-state value-based care organization managing Medicare Advantage and ACO REACH populations. They needed RAF optimization that could scale across 245 providers while maintaining audit-ready accuracy.
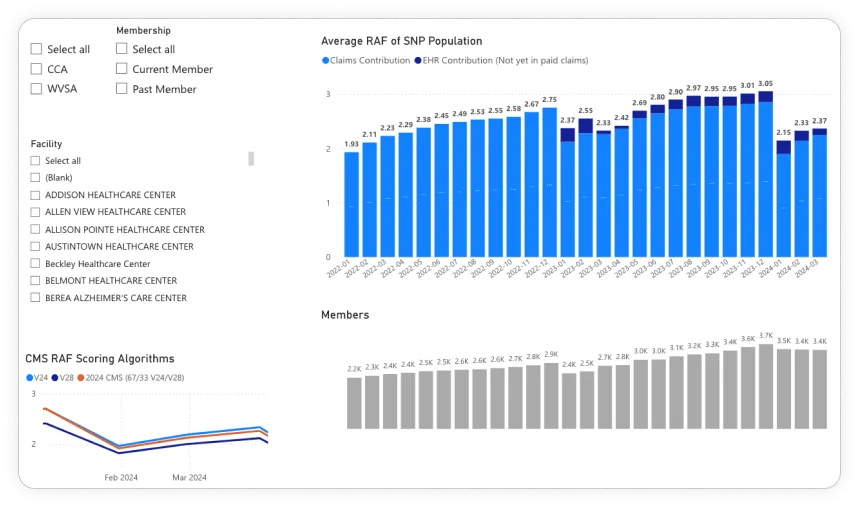
HCC Recapture Rate
Improved annual recapture of known chronic conditions from 60-65% to 85-90%-closing the documentation gap.
Suspected Conditions
Identified 15-20% additional HCC opportunities from clinical evidence that hadn't been formally diagnosed.
Audit Performance
Documentation linkage and explainability enabled confident audit defense with minimal findings.
Integrated with PointClickCare, Gehrimed, Acclivity, and more.
Our RAF platform integrates with the EHR systems value-based care organizations actually use. We pull clinical documentation, labs, medications, and claims data-creating a holistic patient view that manual review can't match.
Recommendations flow back into provider workflows at the point of care. Alerts before visits, embedded decision support during documentation, and tracking dashboards for population management.
For organizations with multiple EHRs across their network, we handle the complexity-normalizing data from different sources into unified RAF insights.
Production Integrations
PointClickCare
Primary SNF/PAC integration for long-term care populations
Gehrimed
Post-acute care physician practice management
Acclivity
Healthcare software platform integration
Claims Data
Integration with CMS claims for prior-year HCC history
Lab Systems
Direct lab result integration for clinical evidence
RAF optimization often combines with these domains.
Value-Based Care
RAF accuracy directly impacts VBC benchmarks and ACO REACH performance targets.
Learn more →MDS / PDPM
MDS assessments and HCC coding target the same chronic conditions. Unified approach maximizes capture.
Learn more →Documentation Automation
Better clinical documentation creates the evidence RAF optimization needs.
Learn more →Ambient AI Scribes
AI scribes capture diagnoses and clinical detail that improve HCC code specificity.
Learn more →Revenue Cycle AI
Accurate risk adjustment feeds directly into claims and reimbursement optimization.
Learn more →Frequently Asked Questions
Common questions about RAF/HCC coding optimization and AI-powered risk adjustment.
AI frameworks that power this domain.
Ready to optimize your risk adjustment?
30-minute call. We'll assess your RAF opportunity based on population size, current recapture rates, and payer mix.
Assess Your RAF OpportunityOr call: 404.654.3855
Related Insights
From Our Blog

Leveraging AI tools in Social Need Screening and Intervention – comments on proposed changes to HEDIS SNS-E measure
Feb 19, 2025

AI & The Job Landscape, ChatGPT’s Role, & The Future of RPM
Dec 12, 2023
Leveraging AI for ROI in Healthcare: 10 Custom Solutions for 2026
Nov 28, 2025