45-day revenue cycles. 12% denial rates. Back-office is bleeding you dry.
50% of AI budgets go to sales and marketing. But back-office automation delivers the fastest, clearest ROI. Revenue cycle, coding, scheduling, intake-these are the workflows where AI agents create hard dollar returns within the calendar year.
Days Revenue Cycle
Denial Rate Reduction
EBITDA bps Improvement
Admin Cost Reduction
Administrative overhead is eating your margins.
Revenue cycle length
Cash tied up in A/R while you wait. Working capital that could be deployed elsewhere. And the longer claims age, the less likely you are to collect.
Denial rates
Every denial is revenue delayed or lost. Appeals take staff time. Many denials are preventable with better front-end processes and coding accuracy.
Admin overhead
Back-office costs consuming margin. Manual processes that don't scale. Staff doing repetitive work that should be automated.
AI agents that work your back-office 24/7.
Intelligent agents that handle revenue cycle tasks, coding assistance, scheduling optimization, and intake processing. Not chatbots-actual workflow automation that processes transactions, makes decisions, and escalates exceptions.
These agents learn your specific payer rules, contract terms, and denial patterns. They prioritize A/R based on collectability. They catch coding errors before claims go out. They identify the 12% of claims likely to deny-before you submit them.
Built for your environment and trained on your data. Your payer mix. Your EHR. Your workflows. Not a generic tool that requires you to change how you work-AI that learns how you actually operate and gets smarter every month.
Back-office beats front-office for AI ROI.
Industry data shows 50% of AI budgets go to sales and marketing. But back-office automation delivers faster payback and clearer cost reduction. Why?
Front-office AI:
Theoretical revenue gains. Hard to measure. Long feedback loops. Success depends on customer behavior you don't control.
Back-office AI:
Direct cost reduction. Measurable from day one. Short feedback loops. Success depends on processes you control. $2-10M annually in BPO elimination potential.
Where back-office AI delivers.
Revenue Cycle Management
A/R prioritization based on collectability scoring. Denial prediction before submission. Automated appeals for common denial patterns. Contract term interpretation for billing accuracy.
Impact: 45→28 days, millions in faster collections
RAF / HCC Coding
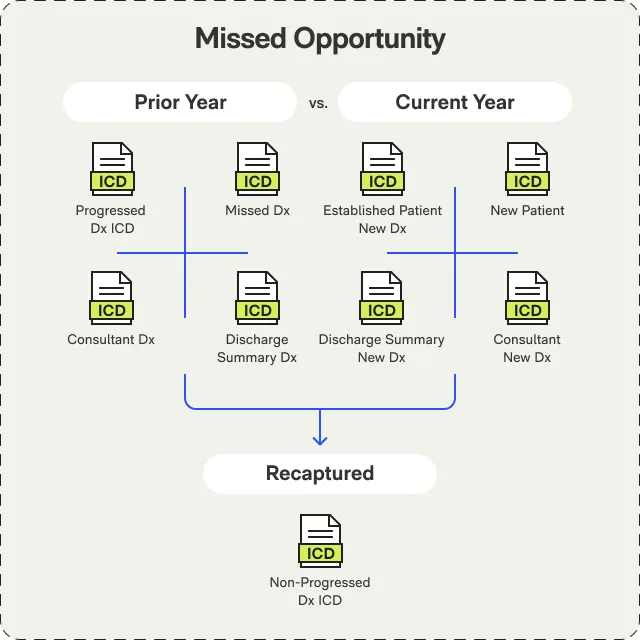
Risk adjustment accuracy for Medicare Advantage and value-based care. Documentation gaps identified. Diagnosis recommendations with supporting evidence. Higher ICD/HCC recapture rates.
Impact: $10M+ improvements, 90%+ accuracy
Scheduling & Capacity
Predictive no-show management with automated fill. Route optimization for home health. Patient acuity matching to staff capabilities. Capacity utilization optimization.
Impact: 15% visit completion improvement, 20% less drive time
Intake & Eligibility
Insurance verification automation. Prior authorization status tracking. Assessment scheduling coordination. Referral source management and follow-up.
Impact: Faster admissions, fewer coverage surprises
Back-office results we've delivered.
CommuniCare Health Services
PDPM Revenue (2 states, annualized)
Quality Incentives
AI-assisted MDS assessment tool that identifies documentation gaps, suggests diagnosis codes, and optimizes PDPM scoring. Financial analyst validated ROI.
RAF / HCC Coding Platform
Risk Adjustment Improvements
Diagnosis Accuracy
20K+ patients, 7 states, 245 providers. Peer-reviewed CMS models. Every recommendation linked to source documentation. Audit-defensible.
EBITDA improvement you can measure.
Revenue Cycle Impact
Faster A/R turns = better working capital. Reduced denials = higher net collections. Contract compliance = capturing what you're owed.
200-300 bps EBITDA
Cost Reduction
Reduced administrative staff requirements. BPO elimination potential. Lower external agency spend.
30-40% admin reduction
Risk Adjustment
Higher RAF scores = higher MA payments. Better HCC capture = accurate risk profiles. Audit-defensible documentation.
$10M+ improvement potential
See how back-office AI applies to your revenue cycle.
30-minute discovery call to understand your back-office challenges and quantify the opportunity. Calendar year ROI is possible.
Schedule AI Opportunity AssessmentRelated Insights
From Our Blog

Two Years of Using AI in Software Engineering: A Personal Retrospective
Jun 26, 2025

Healthcare Revenue Optimization: How AI Helped a Post-Acute Care Provider Generate $12M+
Mar 03, 2025

An Essential Guide to Managing Software Development Risk and Maximizing ROI
Dec 23, 2025