Revenue Cycle AI
Downstream RCM tools are getting better at processing what they receive—that problem is increasingly solved. The unsolved problem is upstream: clinical documentation, coding specificity, medical necessity alignment, and payer policy mismatch. We build the intelligence layer that fixes revenue at the source.
Verified ROI
Days in A/R
Denial Rate
bps EBITDA
Every denial costs $25–$118 to rework. Providers blow past alerts.
McKinsey estimates that AI enablement of healthcare revenue cycle could cut cost to collect by 30–60%. Nearly 20% of claims are denied on average; as many as 60% of those are never appealed—representing millions in preventable lost revenue.
Quality Gap
Clinical documentation, coding specificity, and medical necessity alignment are where revenue is lost—before a claim is ever submitted.
Clinical ↔ Financial
A physician ordering a procedure doesn’t know the denial rate for that order with that specific payer. Clinical decisions and financial consequences live in separate systems.
Alert Overload
Providers dismiss alerts because they create friction without providing value. The better path has to be the easier path—or adoption will never happen.
Three layers, one system.
We don’t bolt AI onto your existing RCM stack. We build an intelligence layer that learns your specific payer mix, fights your specific denial patterns, and becomes an institutional capability you own.
Data Audit
Map where leakage happens. Pareto analysis of denial drivers by denied dollars—not count. Quantified, prioritized foundation for every decision that follows.
See the Revenue Integrity Audit →Data Engineering
Clean and connect inputs so claims start cleaner before anyone touches them. Patient identity, eligibility, authorization linkage, payer rules. Fix the plumbing—denials disappear.
Workflow Intelligence
Surface contextual insights to providers at point of work. Light touch: supporting evidence, no hard stops. Providers adopt it because it makes work easier, not harder.
Light touch, provider-driven.
Make the better path the easier path
Reduce cognitive load, not add it
Let providers validate and own changes
Documentation–to–revenue visibility
Use subtle organizational incentives
Peer benchmarking, RVU alignment
Never get in the way of patient care
Contextual, non-interruptive, trust-building
Financial analyst-calculated ROI. Not vendor estimates. $20M+ verified.
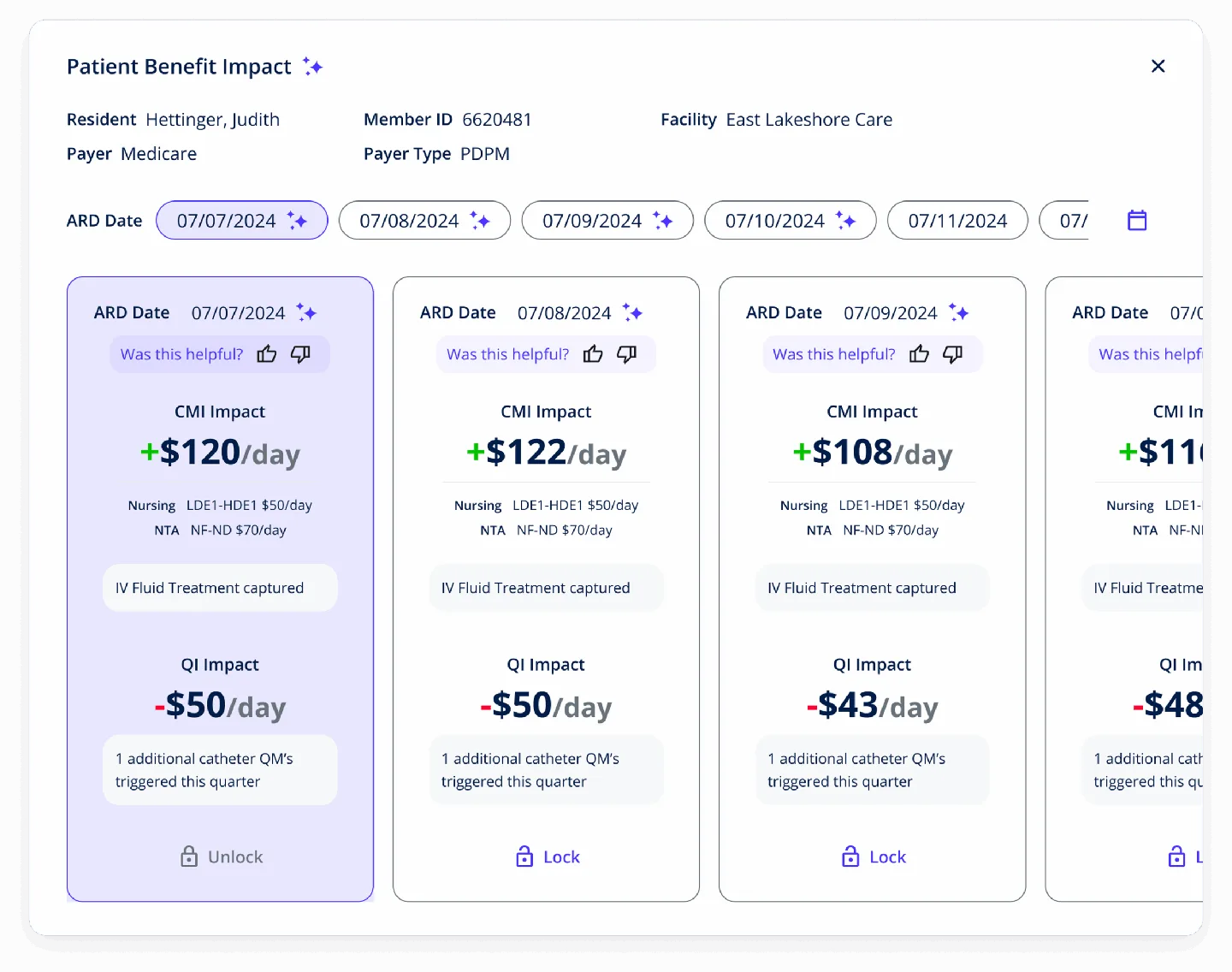
$10M+ PDPM Revenue Recovered
AI-powered MDS assessment optimization for one of the nation’s largest post-acute care providers. 95% reduction in assessment discrepancies. EHR-native PointClickCare integration.
PDPM Revenue
Quality Incentives
Time Savings
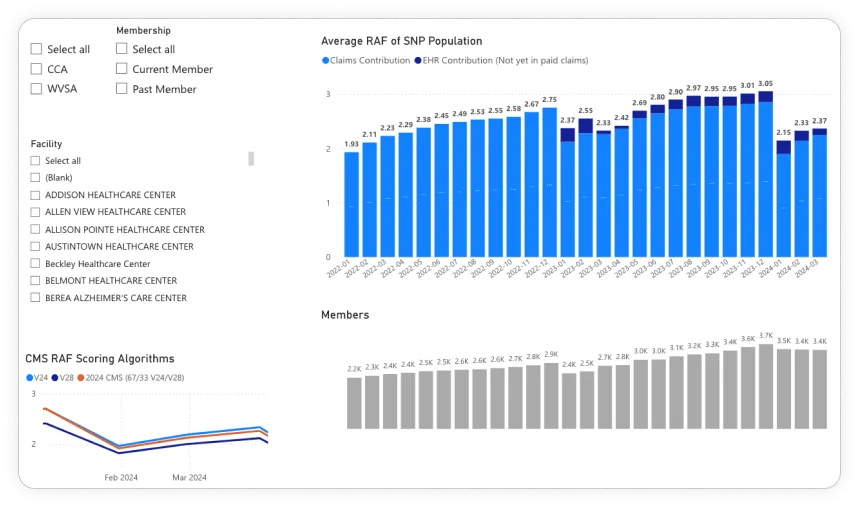
$12M Recurring Annual Revenue
AI-powered medical coding that reviews patients 50x faster than manual audit. 98% clinician adoption. Built in 12 weeks, ROI in 4 months.
Annual Revenue
20K+ Patients
Clinician Adoption
Revenue Integrity Data Audit
Before we build anything, we map where your revenue is leaking—and quantify how much you can recover.
What You Get
Revenue Cycle Health Scorecard
Denial rate, clean claim rate, A/R days by payer, facility, and provider
Denial Taxonomy
CARC/RARC codes normalized to root-cause buckets
Pareto Analysis
Top 10 denial buckets ranked by denied dollars—not count
Opportunity Ranking
Scored by dollar impact, preventability, and data readiness
Intelligence Layer Briefs
Top 3–5 AI intervention opportunities with expected ROI
60–90 Day Pilot Plan
Tied to the highest-ROI opportunity your finance team will accept
Revenue cycle intelligence we’ve built.
Works with your existing systems
Revenue cycle AI requires deep integration with billing systems, EHRs, and clearinghouses. We have production experience with the platforms you use.
Practice Management
Integration with PM systems for claims, patient demographics, and payment posting.
EHR Systems
PointClickCare, Epic, Gehrimed, Elation—bidirectional data flows for clinical context.
Clearinghouses
Claims submission, status tracking, 835 ERA processing, and denial feed ingestion.
Payer Portals
Automated eligibility checks, prior auth status, plan-level coverage rules, and claims inquiry.
We don’t just build and hand off. We operate, support, and stand behind our work.
Discover
Data Foundation — Ingest 12–18 months of claims + remittance data, map denial patterns
Solution Design — Revenue Integrity Audit, Pareto analysis, opportunity ranking by denied dollars
Experiment
Hypothesis & Scope — Target highest-ROI denial bucket with pilot intelligence layer
Build & Validate — Working AI tested on real claims data with operational feedback
Engineer
Agile Development — Iterative sprints with RCM team feedback
Systems Integration — EHR, clearinghouse, and payer portal connections
Change Management — Provider training, workflow adoption
Production Deploy — Phased rollout with monitoring
Optimize
KPI Accountability — Revenue impact validated by independent financial analyst
Continuous Improvement — Model retraining, payer policy updates, ongoing support
Often combined with
MDS / PDPM Optimization
Accurate MDS assessments drive PDPM reimbursement upstream.
Learn more →RAF / HCC Coding
Risk adjustment accuracy directly impacts revenue for VBC organizations.
Learn more →Intelligent Back-Office Agents
Revenue cycle AI is part of our broader back-office automation framework.
See framework →Ambient AI Scribes
Complete documentation at the point of care means cleaner claims downstream.
Learn more →EHR Integrations
Revenue cycle automation requires deep integration with clinical and billing systems.
Learn more →Frequently Asked Questions
Common questions about AI-powered revenue cycle management for healthcare organizations.
AI frameworks that power this domain.
Ready to quantify your upstream revenue opportunity?
Start with a Revenue Integrity Data Audit. 2–4 weeks. We’ll show you exactly where revenue is leaking and what AI can recover.
Or call: 404.654.3855
Related Insights
From Our Blog

Leveraging AI tools in Social Need Screening and Intervention – comments on proposed changes to HEDIS SNS-E measure
Feb 19, 2025

AI & The Job Landscape, ChatGPT’s Role, & The Future of RPM
Dec 12, 2023
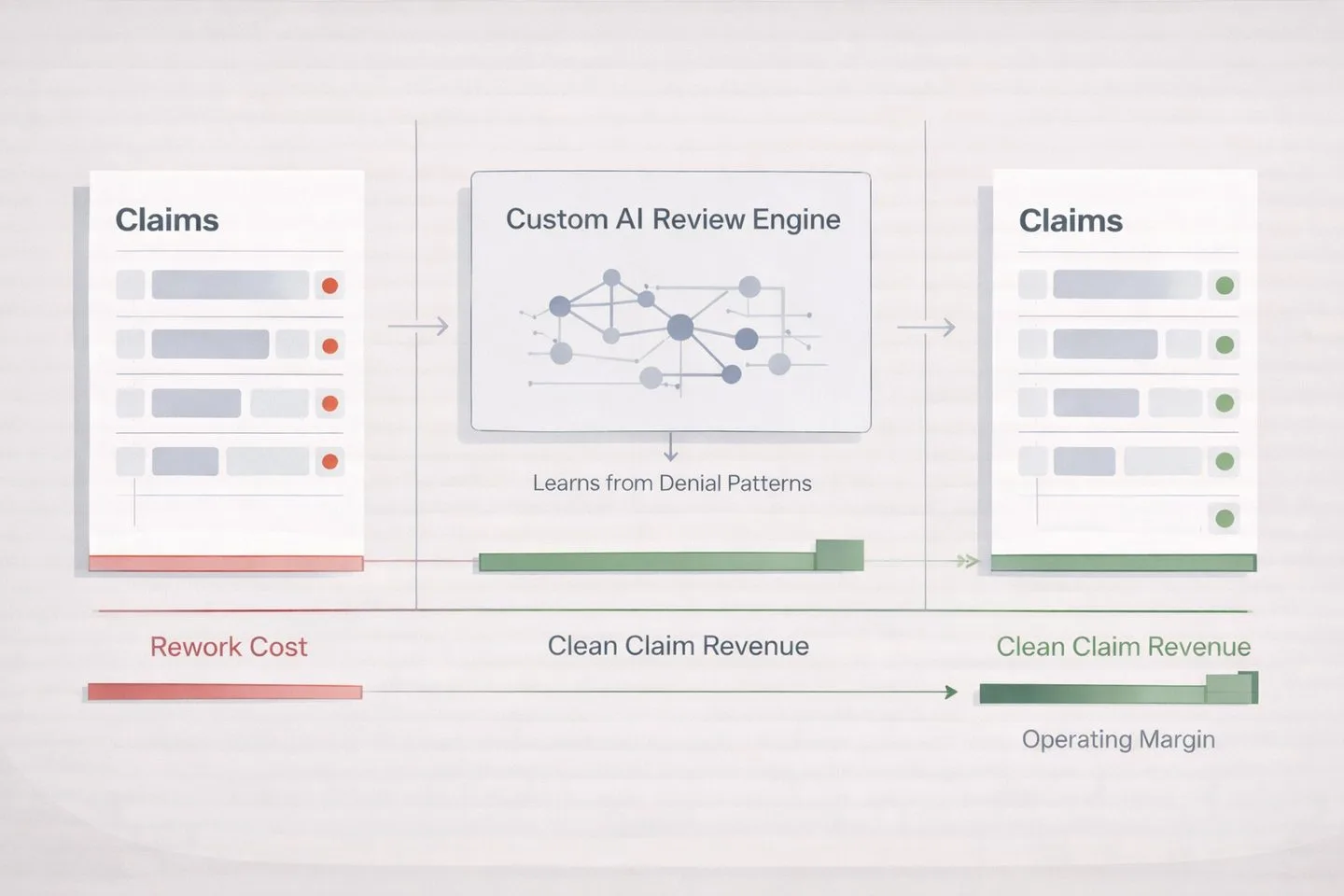
Leveraging AI for ROI in Healthcare: 10 Custom Solutions for 2026
Nov 28, 2025